|
Adminஐﻬ
|
 |
« on: February 10, 2006, 10:30:52 pm » |
|
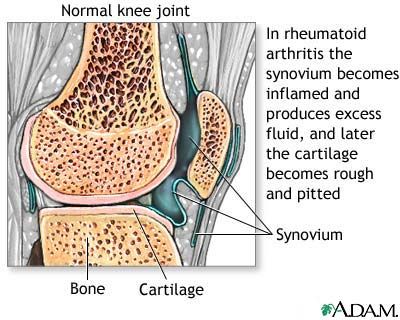
Rheumatoid arthritis
Overview
The nagging pains and physical limitations of the more than 100 forms of arthritis are common to millions of people. Rheumatoid arthritis is among the most debilitating of all forms, causing joints to ache and throb and eventually become deformed. Sometimes these symptoms make even the simplest activities such as opening a jar or taking a walk difficult to manage.
Unlike osteoarthritis, which results from wear and tear on your joints, rheumatoid arthritis is an inflammatory condition. The exact cause of rheumatoid arthritis is unknown, but it's believed to be the body's immune system attacking the tissue that lines your joints (synovium).
Rheumatoid arthritis is two to three times more common in women than in men and generally strikes between the ages of 20 and 50. But rheumatoid arthritis can also affect young children and adults older than age 50.
There's no cure for rheumatoid arthritis. But with proper treatment, a strategy for joint protection and changes in lifestyle, you can live a long, productive life with this condition.
Signs and symptoms
The signs and symptoms of rheumatoid arthritis may come and go over time. They include:
Pain and swelling in your joints, especially in the smaller joints of your hands and feet
Generalized aching or stiffness of the joints and muscles, especially after sleep or after periods of rest
Loss of motion of the affected joints
Loss of strength in muscles attached to the affected joints
Fatigue, which can be severe during a flare-up
Low-grade fever
Deformity of your joints over time
General sense of not feeling well (malaise)
Rheumatoid arthritis usually causes problems in several joints at the same time. Early in rheumatoid arthritis, the joints in your wrists, hands, feet and knees are the ones most often affected. As the disease progresses, your shoulders, elbows, hips, jaw and neck can become involved. It generally affects both sides of your body at the same time. The knuckles of both hands are one example.
Small lumps, called rheumatoid nodules, may form under your skin at pressure points and can occur at your elbows, hands, feet and Achilles tendons. Rheumatoid nodules may also occur elsewhere, including the back of your scalp, over your knee or even in your lungs. These nodules can range in size from as small as a pea to as large as a walnut. Usually these lumps aren't painful.
In contrast to osteoarthritis, which affects only your bones and joints, rheumatoid arthritis can cause inflammation of tear glands, salivary glands, the linings of your heart and lungs, your lungs themselves and, in rare cases, your blood vessels.
Although rheumatoid arthritis is often a chronic disease, it tends to vary in severity and may even come and go. Periods of increased disease activity called flare-ups or flares alternate with periods of relative remission, during which the swelling, pain, difficulty sleeping, and weakness fade or disappear.
Swelling or deformity may limit the flexibility of your joints. But even if you have a severe form of rheumatoid arthritis, you'll probably retain flexibility in many joints.
Causes
As with other forms of arthritis, rheumatoid arthritis involves inflammation of the joints. A membrane called the synovium lines each of your movable joints. When you have rheumatoid arthritis, white blood cells whose usual job is to attack unwanted invaders, such as bacteria and viruses move from your bloodstream into your synovium. Here, these blood cells appear to play an important role in causing the synovial membrane to become inflamed (synovitis).
This inflammation results in the release of proteins that, over months or years, cause thickening of the synovium. These proteins can also damage cartilage, bone, tendons and ligaments. Gradually, the joint loses its shape and alignment. Eventually, it may be destroyed.
Some researchers suspect that rheumatoid arthritis is triggered by an infection possibly a virus or bacterium in people with an inherited susceptibility. Although the disease itself is not inherited, certain genes that create an increased susceptibility are. People who have inherited these genes won't necessarily develop rheumatoid arthritis. But they may have more of a tendency to do so than others. The severity of their disease may also depend on the genes inherited. Some researchers also believe that hormones may be involved in the development of rheumatoid arthritis.
Risk factors
The exact causes of rheumatoid arthritis are unclear, but these factors may increase your risk:
Getting older, because incidence of rheumatoid arthritis increases with age. However, incidence begins to decline in women over the age of 80.
Being female.
Being exposed to an infection, possibly a virus or bacterium, that may trigger rheumatoid arthritis in those with an inherited susceptibility.
Inheriting specific genes that may make you more susceptible to rheumatoid arthritis.
Smoking cigarettes over a long period of time.
When to seek medical advice
See your doctor if you have persistent discomfort and swelling in multiple joints on both sides of your body. Your doctor can work with you to develop a pain management and treatment plan. Also seek medical advice if you experience side effects from your arthritis medications. Side effects may include nausea, abdominal discomfort, black or tarry stools, changes in bowel habits, constipation and drowsiness.
Screening and diagnosis
If you have signs and symptoms of rheumatoid arthritis, your doctor will likely conduct a physical examination and request laboratory tests to determine if you have this form of arthritis. These tests may include:
Blood tests. A blood test that measures your erythrocyte sedimentation rate (ESR or sed rate) can indicate the presence of an inflammatory process in your body. People with rheumatoid arthritis tend to have elevated ESRs. The ESRs in those with osteoarthritis tend to be normal.
Another blood test looks for an antibody called rheumatoid factor. Most people with rheumatoid arthritis eventually have this abnormal antibody, although it may be absent early in the disease. It's also possible to have the rheumatoid factor in your blood and not have rheumatoid arthritis.
Imaging. Doctors may take X-rays of your joints to differentiate between osteoarthritis and rheumatoid arthritis. A sequence of X-rays obtained over time can show the progression of arthritis.
Complications
Rheumatoid arthritis causes stiffness and pain and may also cause fatigue. It can lead to difficulty with everyday tasks, such as turning a doorknob or holding a pen. Dealing with the pain and the unpredictability of rheumatoid arthritis can also cause symptoms of depression.
Rheumatoid arthritis may also increase your risk of developing osteoporosis, especially if you take corticosteroids. Some researchers believe that rheumatoid arthritis can increase your risk of heart disease. This may be because the inflammation that rheumatoid arthritis causes can also affect your arteries and heart muscle tissue.
In the past, people with rheumatoid arthritis may have ended up confined to a wheelchair because damage to joints made it difficult or impossible to walk. That's not as likely today because of better treatments and self-care methods.
Treatment
Treatments for arthritis have improved in recent years. Most treatments involve medications. But in some cases, surgical procedures may be necessary.
Medications
Medications for rheumatoid arthritis can relieve its symptoms and slow or halt its progression. They include:
Nonsteroidal anti-inflammatory drugs (NSAIDs). This group of medications, which includes aspirin, helps relieve both pain and inflammation if you take the drugs regularly. NSAIDs that are available over-the-counter include aspirin, ibuprofen (Advil, Motrin, others) and naproxen sodium (Aleve).
These are available at higher dosages, and other NSAIDs are available by prescription such as ketoprofen, naproxen (Anaprox, Naprosyn), tolmetin (Tolectin), diclofenac (Voltaren), nabumetone (Relafen) and indomethacin (Indocin). Taking NSAIDs can lead to side effects such as indigestion and stomach bleeding. Other potential side effects may include damage to the liver and kidneys, ringing in your ears (tinnitus), fluid retention and high blood pressure. NSAIDs, except aspirin, may also increase your risk of cardiovascular events such as heart attack or stroke.
COX-2 inhibitors. This class of NSAIDs may be less damaging to your stomach. Like other NSAIDs, COX-2 inhibitors such as celecoxib (Celebrex) suppress an enzyme called cyclooxygenase (COX) that's active in joint inflammation. Other types of NSAIDs work against two versions of the COX enzyme that are present in your body: COX-1 and COX-2.
However, there's evidence that by suppressing COX-1, NSAIDs may cause stomach and other problems because COX-1 is the enzyme that protects your stomach lining. Unlike other NSAIDs, COX-2 inhibitors suppress only COX-2, the enzyme involved in inflammation. Side effects may include fluid retention and causing or exacerbating high blood pressure. Furthermore, this class of drugs has been linked to an increased risk of heart attack and stroke.
Corticosteroids. These medications, such as prednisone and methylprednisolone (Medrol), reduce inflammation and pain, and slow joint damage. In the short term, corticosteroids can make you feel dramatically better. But when used for many months or years, they may become less effective and cause serious side effects. Side effects may include easy bruising, thinning of bones, cataracts, weight gain, a round face and diabetes. Doctors often prescribe a corticosteroid to relieve acute symptoms, with the goal of gradually tapering off the medication.
Disease-modifying antirheumatic drugs (DMARDs). Physicians prescribe DMARDs to limit the amount of joint damage that occurs in rheumatoid arthritis. Taking these drugs at early stages in the development of rheumatoid arthritis is especially important in the effort to slow the disease and save the joints and other tissues from permanent damage. Because many of these drugs act slowly it may take weeks to months before you notice any benefit DMARDs typically are used with an NSAID or a corticosteroid.
While the NSAID or corticosteroid handles your immediate symptoms and limits inflammation, the DMARD goes to work on the disease itself. Some commonly used DMARDs include hydroxychloroquine (Plaquenil), the gold compound auranofin (Ridaura), sulfasalazine (Azulfidine), minocycline (Dynacin, Minocin) and methotrexate (Rheumatrex). Other forms of DMARDs include immunosuppressants and tumor necrosis factor (TNF) blockers.
Immunosuppressants. These medications act to tame your immune system, which is out of control in rheumatoid arthritis. In addition, some of these drugs attack and eliminate cells that are associated with the disease. Some of the commonly used immunosuppressants include leflunomide (Arava), azathioprine (Imuran), cyclosporine (Neoral, Sandimmune) and cyclophosphamide (Cytoxan). These medications can have potentially serious side effects such as increased susceptibility to infection.
TNF blockers. These are a class of DMARDs known as biologic response modifiers. TNF is a cytokine, or cell protein, that acts as an inflammatory agent in rheumatoid arthritis. TNF blockers, or anti-TNF medications, target or block this cytokine and can help reduce pain, morning stiffness and tender or swollen joints usually within one or two weeks after treatment begins. There is evidence that TNF blockers may halt progression of disease. These medications often are taken with methotrexate.
TNF blockers approved for treatment of rheumatoid arthritis are etanercept (Enbrel), infliximab (Remicade) and adalimumab (Humira). Potential side effects include injection site irritation (adalimumab and etanercept), worsening congestive heart failure (infliximab), blood disorders, lymphoma, demyelinating diseases, and increased risk of infection. If you have an active infection, don't take these medications.
Interleukin-1 receptor antagonist (IL-1Ra). IL-1Ra is another type of biologic response modifier and is a recombinant form of the naturally occurring interleukin-1 receptor antagonist (IL-1Ra). Interleukin-1 (IL-1) is a cell protein that promotes inflammation and occurs in excess amounts in people who have rheumatoid arthritis or other types of inflammatory arthritis. If IL-1 is prevented from binding to its receptor, the inflammatory response decreases.
The first IL-1Ra that has been approved by the Food and Drug Administration for use in people with moderate to severe rheumatoid arthritis who haven't responded adequately to conventional DMARD therapy is anakinra (Kineret). It may be used alone or in combination with methotrexate. Anakinra is given as a daily self-administered injection under the skin. Some potential side effects include injection site reactions, decreased white blood cell counts, headache and an increase in upper respiratory infections. There may be a slightly higher rate of respiratory infections in people who have asthma or chronic obstructive pulmonary disease. If you have an active infection, don't use anakinra.
Antidepressant drugs. Some people with arthritis also experience symptoms of depression. The most common antidepressants used for arthritis pain and nonrestorative sleep are amitriptyline, nortriptyline (Aventyl, Pamelor) and trazodone (Desyrel).
Surgical or other procedures
Although a combination of medication and self-care is the first course of action for rheumatoid arthritis, other methods are available for severe cases:
Prosorba column. This blood-filtering technique removes certain antibodies that contribute to pain and inflammation in your joints and muscles and is usually performed once a week for 12 weeks as an outpatient procedure. Some of the side effects include fatigue and a brief increase in joint pain and swelling for the first few days after the treatment.
The Prosorba column treatment isn't recommended if you're taking angiotensin-converting enzyme (ACE) inhibitors or if you have heart problems, high blood pressure or blood-clotting problems.
Joint replacement surgery. For many people with rheumatoid arthritis, medicines and therapies can't prevent joint destruction. When joints are severely damaged, joint replacement surgery can often help restore joint function, reduce pain or correct a deformity.
You may need to have an entire joint replaced with a metal or plastic prosthesis. Surgery may also involve tightening tendons that are too loose, loosening tendons that are too tight, fusing bones to reduce pain or removing part of a diseased bone to improve mobility. Your doctor may also remove the inflamed joint lining (synovectomy).
Self-care
Treating rheumatoid arthritis typically involves using a combination of medical treatments and self-care strategies. The following self-care procedures are important elements for managing the disease:
Exercise regularly. Different types of exercise achieve different goals. Check with your doctor or physical therapist first and then begin a regular exercise program for your specific needs. If you can walk, walking is a good starter exercise. If you can't walk, try a stationary bicycle with little or no resistance or do hand or arm exercises. A chair exercise program may be helpful. Aquatic exercise is another option, and many health clubs with pools offer such classes.
It's good to move each joint in its full range of motion every day. As you move, maintain a slow, steady rhythm. Don't jerk or bounce. Also, remember to breathe. Holding your breath can temporarily deprive your muscles of oxygen and tire them. It's also important to maintain good posture while you exercise.
Avoid exercising tender, injured or severely inflamed joints. If you feel new joint pain, stop. New pain that lasts more than two hours after you exercise probably means you've overdone it. If pain persists for more than a few days, call your doctor.
Control your weight. Excess weight puts added stress on joints in your back, hips, knees and feet the places where arthritis pain is commonly felt. Excess weight can also make joint surgery more difficult and risky.
Eat a healthy diet. A healthy diet emphasizing fruit, vegetables and whole grains can help you control your weight and maintain your overall health, allowing you to deal better with your arthritis. However, there's no special diet that can be used to treat arthritis. It hasn't been proved that eating any particular food will make your joint pain or inflammation better or worse.
Apply heat. Heat will help ease your pain, relax tense, painful muscles and increase the regional flow of blood. One of the easiest and most effective ways to apply heat is to take a hot shower or bath for 15 minutes. Other options include using a hot pack, an electric heat pad set on its lowest setting or a radiant heat lamp with a 250-watt reflector heat bulb to warm specific muscles and joints.
If your skin has poor sensation or if you have poor circulation, don't use heat treatment.
Apply cold for occasional flare-ups. Cold may dull the sensation of pain. Cold also has a numbing effect and decreases muscle spasms. Don't use cold treatments if you have poor circulation or numbness. Techniques may include using cold packs, soaking the affected joints in cold water and ice massage.
Practice relaxation techniques. Hypnosis, guided imagery, deep breathing and muscle relaxation can all be used to control pain.
Take your medications as recommended. By taking medications regularly instead of waiting for pain to build, you will lessen the overall intensity of your discomfort.
Coping skills
The degree to which rheumatoid arthritis affects your daily activities depends in part on how well you cope with the disease. Physical and occupational therapists can help you devise strategies to cope with specific limitations you may experience as the result of weakness or pain.
|
|
|
|
« Last Edit: May 17, 2006, 05:41:13 pm by Kathy »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #1 on: March 06, 2006, 10:33:36 pm » |
|
American Rheumatism Association Criteria for the Classification of Rheumatoid Arthritis
Criteria
Morning stiffness:morning stiffness in and around the joints lasting at least 1 hr before maximal improvement
Arthritis of three or more joint areas: at least three joint areas have simultaneously had soft tissue swelling or fluid (not bony overgrowth alone) observed by a physician; the 14 possible joint areas (right and left) are proximal interphalangeal (PIP), metacarpophalangeal (MCP), wrist, elbow, knee, ankle, and metatarsophalangeal (MTP) joints
Arthritis of hand joints: at least one joint area swollen as above in wrist, MCP, or PIP joint
Symmetrical arthritis: simultaneous involvement of the same joint areas (as in arthritis of three or more joint areas, above) on both sides of the body (bilateral involvement of PIP, MCP, or MTP joints is acceptable without absolute symmetry)
Rheumatoid nodules: subcutaneous nodules over bony prominences or extensor surfaces or in juxta-articular regions that are observed by a physician
Serum rheumatoid factor: demonstration of abnormal amounts of serum rheumatoid factor by any method that has been positive in fewer than 5% of normal control subjects
Radiographic changes: radiographic changes typical of rheumatoid arthritis on posteroanterior hand and wrist x-rays, which must include erosions or unequivocal bony decalcification localized to or most marked adjacent to the involved joints (osteoarthritis changes alone do not qualify)
Exclusions
The presence of any of the following excludes the diagnosis of rheumatoid arthritis:
Typical rash of systemic lupus erythematosus (SLE)
High concentration of lupus erythematosus cells (four or more in two smears); because of the frequent finding of LE cells in patients with clinically typical rheumatoid arthritis, however, it is suggested that such patients be listed separately
Histologic evidence of polyarteritis nodosa with segmented necrosis of arteries associated with nodular leukocytic infiltration extending perivascularly, including many eosinophils
Persistent muscle swelling of dermatomyositis or weakness of neck, trunk, and pharyngeal muscles
Definite scleroderma (not limited to the fingers)
A clinical picture characteristic of rheumatic fever with migratory joint involvement and evidence of endocarditis, especially if accompanied by subcutaneous nodules, erythema marginatum, or chorea (an elevated antistreptolysin titer will not rule out the diagnosis of rheumatoid arthritis)
A clinical picture characteristic of gouty arthritis with acute attacks of swelling, redness, and pain in one or more joints, especially if responsive to colchicine
Tophi
A clinical picture characteristic of acute infectious arthritis of bacterial or viral origin with an acute focus of infection or a close association with a disease of known infectious origin; chills; fever; acute joint involvement, usually initially migratory (especially if organisms are present in the joint fluid or there is a response to antibiotic therapy)
Tubercle bacilli in joints or histologic evidence of joint tuberculosis
A clinical picture characteristic of reactive arthritis with urethritis and conjunctivitis associated with acute joint involvement, usually initially migratory
A clinical picture characteristic of the shoulder-hand syndrome with unilateral involvement of shoulder and hand and diffuse swelling of the hand, followed by atrophy and contractures
A clinical picture characteristic of hypertrophic osteoarthropathy with clubbing of fingers or hypertrophic periostitis, or both, along the shafts of the long bones, especially if an intrapulmonary lesion is present
A clinical picture characteristic of neuroarthropathy with condensation and destruction of bones of involved joints and associated neurologic findings
Homogentisic acid in the urine grossly detectable by alkalinization
Histologic evidence of sarcoid or a positive Kveim test
Multiple myeloma evidenced by marked increase in plasma cells in the bone marrow or by Bence Jones protein in the urine
Characteristic skin lesions of erythema nodosum
Leukemia or lymphoma with characteristic cells in peripheral blood, bone marrow, or tissues
A clinical picture characteristic of ankylosing spondylitis, psoriasis, ulcerative colitis, or regional enteritis
Note: for classification purposes, a patient is said to have rheumatoid arthritis if he or she has satisfied at least four of the above seven criteria. The first four must be present for at least 6 wk. Patients with two clinical diagnoses are not excluded. Designation as classic, definite, or probable rheumatoid arthritis is not to be made.
Table 2. Comparison of Various Antirheumatic Treatments
Drug Response Rate; Onset of Action Magnitude of Efficacy (0 to ++++) Major Toxicities Dosage
Anakinra 30%; 1-3 mo + to ++ Injection site reactions, infections 100 mg/day S.C.
Azathioprine 30%-50%; 2-3 mo ++ Hematologic, immunosuppression, cholestasis 100-150 mg/day
Cyclosporine 30%; 2-3 mo ++ Renal (irreversible), hypertension, hypertrichosis, immunosuppression 2.5-5.0 mg/kg/day
Etanercept 50%-70%; 2-4 wk +++ Injection-site reaction, ?immune surveillance 25 mg S.C. twice a week
Gold 30%; 3-6 mo ++ Skin rash, hematologic, renal 5.0 mg/wk I.M. x 6 mo
Hydroxychloroquine 30%-50%; 2-6 mo ++ Retinopathy, myopathy, hyperpigmentation 200 mg b.i.d.
Infliximab 50%-70%; 2-14 wk +++ Increased infection 3 mg/kg I.V. q. 8 wk
Leflunomide 50%; 2-3 mo ++ Liver, teratogen, gastrointestinal, skin rash 100 mg/day x 3, then 20 mg/day
Methotrexate > 70%; 6-8 wk +++ Liver (fibrosis, elevated enzymes), hematologic, oral ulcers 7.5-15 mg/wk
NSAIDs > 75%; < 2 wk + Gastric erosion, renal Varied
Prednisone > 90%; < 1 wk +++ Skin atrophy, cataracts, osteoporosis, avascular necrosis 5.0-7.5 mg/day
Sulfasalazine > 30%; 2-3 mo ++ Dyspepsia, hemolysis in glucose-6-phosphate dehydrogenase deficiency 1 g b.i.d. or t.i.d.
|
|
|
|
« Last Edit: May 17, 2006, 05:40:22 pm by Kathy »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #2 on: April 08, 2006, 09:56:35 am » |
|
 What makes rheumatoid arthritis (RA) different from other kinds of arthritis? What makes rheumatoid arthritis (RA) different from other kinds of arthritis?
Arthritis is a broad term used to refer to more than 100 conditions that can cause joint pain. RA is an autoimmune disease, while osteoarthritis (OA) is a condition of wear and tear. RA affects pairs of joints. OA affects individual ones. RA usually attacks smaller joints like fingers and feet. OA usually attacks larger ones, like hips. RA can cause extreme tiredness. It also causes morning stiffness that improves as the day goes on. With OA, pain and stiffness worsen during the day. As they are separate conditions, it is also possible to have both conditions at the same time.
 How common is RA and who gets it? How common is RA and who gets it?
Rheumatoid arthritis (RA) affects about 1% of the U.S. population - a total of 2.1 million adults - and nearly 75% of those with RA are women. That's more than 7 out of every 10 people diagnosed with RA. RA can start at any age, from childhood to the senior years, but it usually begins in middle adulthood.
 What causes RA? What causes RA?
Despite more than a century of research, scientists have thus far been unable to pinpoint the cause or causes of rheumatoid arthritis (RA). What is known is that RA is an autoimmune disease, that is, the immune system attacks the body's own joints and other organs. What remains to be discovered is exactly what causes this immune system disease. A number of possibilities have been examined. Genes are one, and it has been found that RA is not inherited directly - that is, it is not passed straight from parents to children. Instead, a genetic susceptibility to RA is inherited, and the disease will develop only if activated by a "trigger." Scientists are currently working to identify possible RA triggers. Infection, injury, hormonal changes, and environmental factors are all the subject of current research.
 How quickly can RA progress? How quickly can RA progress?
Over time, inflammation from rheumatoid arthritis (RA) can damage the joints. RA was once thought to advance fairly slowly. But more recent research reveals that it can actually progress quite quickly. RA's damage may begin as early as the first year of the disease, and 7 of every 10 people diagnosed with RA will have joint destruction that can be clearly seen in X-rays within 3 years.
 How is RA treated? How is RA treated?
The medicines that treat rheumatoid arthritis (RA) fall into different categories: The Pain Controllers and The Disease Treaters. The Pain Controllers kill pain but they can't stop your disease from getting worse. (And RA can progress quickly!) Medications like HUMIRA treat the disease and help slow its progression while they also relieve pain. RA brings inflammation that can lead to the destruction of your joints. While many things may be responsible for this inflammation, one of the culprits is a protein called tumor necrosis factor alpha (TNF-α). Recently, scientists discovered that most patients with RA have too much TNF-α. So medicines that block TNF-α can do a lot to reduce the signs and symptoms of RA. HUMIRA resembles antibodies normally found in your body. HUMIRA blocks TNF-α.
 The Pain Controllers The Pain Controllers
The following medications can reduce inflammation, but are not disease-modifying and do not prevent joint destruction. They are usually not used as the only treatment for rheumatoid arthritis (RA).
* NSAIDs (nonsteroidal anti-inflammatory drugs). These include medicines such as Aleve® (naproxen), aspirin, and Motrin® (ibuprofen). They reduce pain and inflammation. Possible side effects: stomach upset, ulcers, and bleeding.
* COX-2 Inhibitors (a specific class of NSAIDs), such as Celebrex® (celecoxib), reduce pain and inflammation, and are less likely to cause stomach upset. Some side effects may include indigestion, diarrhea, and abdominal pain. In rare cases, serious stomach problems, such as bleeding, can occur without warning.
* Steroids (corticosteroids or glucocorticoids), such as prednisone, triamcinolone, and cortisone, ease joint pain, swelling, and other symptoms of RA. Possible side effects: increased appetite, weight gain, and indigestion. Steroids can also cause or worsen diabetes. Other side effects are brittle bones, fragile skin, glaucoma, cataracts, and less immunity to high blood pressure. You may also experience nervousness and restlessness.
 The Disease Treaters The Disease Treaters
* Traditional DMARDs (disease-modifying antirheumatic drugs), such as methotrexate help prevent joint and cartilage damage. They can bring about great improvements in many patients. Possible side effects: skin rashes, mouth sores, stomach upset, kidney problems, blood abnormalities, and more.
* TNF-antagonists (biologic DMARDs) are designed to reduce the symptoms of RA by helping the body's own immune system to slow down the inflammation process. This is what HUMIRA does. Biologic DMARDs, such as HUMIRA, also slow the progression of joint damage. Such medications are injected under the skin or given via an IV. Common side effects: reactions at the site of the injection or infusion, headache and infections.
 If I have RA, from whom should I get treatment? If I have RA, from whom should I get treatment?
While your primary care physician plays an important role in your general health, the rheumatologist is the doctor who specializes in RA. Rheumatologists have the training and experience to prescribe and manage certain RA medications (to find one near you, click here). Other professionals such as nurses, physical or occupational therapists, orthopedic surgeons, psychologists, social workers, and caregivers can help you cope with other aspects of living with RA.
 Do diet and exercise (lifestyle modifications) alleviate RA symptoms? Do diet and exercise (lifestyle modifications) alleviate RA symptoms?
A healthy diet, rest, regular exercise (to build strength, endurance, and mobility), and stress management can always help. Also, losing weight may reduce the amount of stress on your joints.
 Can RA be cured? Or controlled? Can RA be cured? Or controlled?
Although rheumatoid arthritis (RA) cannot be cured at the moment, the inflammation of RA is controllable if recognized and treated aggressively in its early stages.. Scientists all around the world are working around the clock to find a cure. If you'd like additional treatment information, you can visit www.RA.com. |
|
|
|
« Last Edit: May 17, 2006, 05:39:41 pm by Kathy »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #3 on: July 06, 2006, 08:28:18 pm » |
|
Serum Fetal DNA Levels Tied to Rheumatoid Arthritis Improvement During Pregnancy
NEW YORK (Reuters Health) Jun 27 - Women with rheumatoid arthritis (RA) often improve when they are pregnant. An inverse association between serum levels of fetal DNA and disease activity could account for the improvement, and the rapid relapse postpartum, according to a report in the July issue of Arthritis and Rheumatism
Dr. Zhen Yan, from the Fred Hutchinson Cancer Research Center in Seattle, and her associates obtained blood samples from 25 pregnant patients with RA throughout their pregnancies. The cohort included six patients who were diagnosed with juvenile idiopathic arthritis (JIA).
"Group A" was comprised of women who experienced improved symptoms during pregnancy, including 15 adult-onset RA patients and all six patients with JIA. That improvement was either sustained or increased further during the course of gestation, followed by relapse within 3 to 4 months after delivery
The four "Group B" patients did not experience any improvement throughout their pregnancies.
Real-time quantitative PCR was used to measure serum levels of free fetal DNA. Circulating levels reached a median of 24 fetal genomic equivalents per milliliter (gE/mL) during the first trimester, 61 gE/mL in the second trimester, and 199 gE/mL in the third trimester.
The authors found that serum fetal DNA levels were significantly higher in the third trimester among women in Group A as compared with Group B (median 270 gE/mL versus 78 gE/mL, p < 0.001).
By 3 to 4 months after delivery, RA disease recurrence was experienced by 90% of women in Group A, at which time fetal DNA was almost completely gone from the serum.
As noted, there was an inverse association between serum fetal DNA levels and RA disease activity. Dr. Yan's team suggests that fetal DNA may modulate the immune system, perhaps by induction or alteration of the mother's peripheral T cell repertoire.
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #4 on: July 06, 2006, 08:54:12 pm » |
|
Patients With Rheumatoid Arthritis Continue to Benefit From Abatacept for 2 Years
June 26, 2006 (Amsterdam) Patients with rheumatoid arthritis treated with abatacept (Orencia) who had an inadequate response to methotrexate have a slowed course of joint damage after 2 years of treatment, according to a team of investigators from the United States who presented their findings here at the European Congress of Rheumatology of the European League Against Rheumatism (EULAR).
"After 2 years of treatment, we continued to see less radiographic progression in patients initially treated with both abatacept and methotrexate than those originally on placebo and later switched to abatacept," said Henry K. Genant, MD, during a press briefing. He was referring to the extension phase of a placebo-controlled clinical trial, Abatacept in Inadequate responders to Methotrexate (AIM).
"During the second year we saw 70% less progression in such patients," Dr.Genant added. Overall, the radiographic end point of the extension study showed 57% less progression in the patients started on treatment than in the patients switched from placebo and methotrexate. Dr. Genant is a professor emeritus of radiology, medicine, epidemiology, and orthopaedic surgery at the University of California in San Francisco.
Dr. Genant and colleagues wanted to know if the promising effects of abatacept would be durable and whether a difference would be seen between patients in the AIM study who were receiving the investigative regimen and the control group.
The investigative regimen consisted of a fixed dose of abatacept at approximately 10 mg/kg of body weight along with 1 additional disease-modifying antirheumatic drug (DMARD) or placebo and a DMARD. The treated patients received abatacept on days 1, 15, and 29, and every 4 weeks afterward for 1 year. After the double-blind phase, patients were eligible to enter the extension phase, in which all patients received a fixed dose of ~10 mg/kg of abatacept every 4 weeks.
The investigators obtained radiographs of all the patients' hands and feet at randomization and at 1 and 2 years; they also obtained these images if the patients terminated the study early. The investigators used paired radiographs so that independent experts could evaluate them for erosion score, joint-space narrowing score, and the total score. The scorers used the Genant-modified Sharp score to evaluate the images.
Of the original 652 patients in the double-blind trial, 385 in the abatacept group (88.9%) and 162 controls (74.0%) completed the double-blind phase. Then 539 patients continued in the extension phase, of whom data were available for 536 (376 were originally treated with abatacept and 160 were originally control subjects).
Of those originally treated with abatacept, and therefore continuously treated with abatacept for 2 years, the erosion score had increased a mean of 0.84 points over a mean score of 2.05 points at the onset of the extension study. The patients who were originally controls had a mean score of 3.44 at the onset of the extension and at 2 years their scores had increased an average of 1.69.
The joint space narrowing scores increased 0.71 points for the patients continuously receiving abatacept and 1.48 points for those switched from placebo. At the start of the extension, those patients' joint space narrowing scores were 2.12 and 3.90, respectively. The total scores increased 1.55 points for those receiving 2 years of abatacept and 3.17 points for those switched from placebo; their total scores at the start of the extension were 3.65 and 6.96, respectively (P < .001 for erosion score, P < .05 for joint space narrowing score, and P < .01 for total score).
"The patients on 2 years of abatacept had significantly less progression of joint damage than did the switched patients," Dr. Genant said.
"Rheumatologists are particularly concerned about damage to joints and currently we measure it with x-ray progression," said Ian McInnes, MD, in an interview seeking independent commentary. "We know that damage will predict worse function and quality of life later on, so there is an urgency to predict destruction of the joint. With new treatments, we need to consider whether one of the benefits is protection of the joint." Dr. McInnes is a professor of experimental medicine at the University of Glasgow in Scotland, United Kingdom, where he is a consultant rheumatologist at the Glasgow Royal Infirmary. He is also chair of the Scientific Committee for EULAR.
"With [tumor necrosis factoralpha] inhibitors, joint damage is significantly reduced, and therefore the treatment may protect function if the benefit is sustained," Dr. McInnes added. "This study tells us that abatacept may also have some beneficial effects in preventing joint damage.
"Abatacept works by interrupting a discussion that T cells and other leukocytes have in the joints. We think this is upstream from what happens in joints and bones," Dr. McInnes said. "It's important that this immunomodulatory effect can be translated into a reduction in radiographic damage. The importance to the [rheumatology] community is that this is another mechanism of inhibition that can be related to prevention of joint damage, and that's why it's of interest to us."
EULAR 2006: Abstract OP0015. Presented June 22, 2006.
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #5 on: September 15, 2006, 08:16:01 am » |
|
Diagnosis and Treatment of Rheumatoid Arthritis
The diagnosis and treatment of rheumatoid arthritis (RA) is a team effort between the patient and several types of health care professionals. A person can go to his or her family doctor or internist, or to a rheumatologist -- a doctor who specializes in arthritis and other diseases of the joints, bones, and muscles. As treatment progresses, other professionals often help: nurses, physical or occupational therapists, orthopedic surgeons, psychologists, and social workers.
Education is Important
Studies have shown that people who are well informed and participate actively in their own care experience less pain and make fewer visits to the doctor than do other people with RA. It is important to learn about RA and its treatments, exercise and relaxation approaches, patient/health care provider communication skills, and problem solving. Educational and support programs help people understand the disease and reduce their pain, to cope mentally and physically with the disease, and to have a greater sense of control.
Diagnosing Rheumatoid Arthritis
Rheumatoid arthritis can be difficult to diagnose in its early stages. There is no single test for the disease. In addition, symptoms differ from person to person and can be more severe in some people than in others. Also, symptoms can be similar to those of other types of arthritis and joint conditions, and it may take some time for other conditions to be ruled out as possible diagnoses. Finally, the full range of symptoms develops over time, and only a few symptoms may be present in the early stages. As a result, doctors use a variety of tools to diagnose the disease and to rule out other conditions.
Medical history: This is the patient's description of symptoms and when and how they began. Good communication between patient and doctor is especially important here. For example, the patient's description of pain, stiffness, and joint function and how these change over time is critical to the doctor's initial assessment of the disease and his or her assessment of how the disease changes.
Physical examination: This includes the doctor's examination of the joints, skin, reflexes, and muscle strength.
Laboratory tests: One common test is for rheumatoid factor, an antibody that is eventually present in the blood of most RA patients. An antibody is a special protein made by the immune system that normally helps fight foreign substances in the body. Not all people with RA test positive for rheumatoid factor, especially early in the disease. And some others who do test positive never develop the disease. Other common tests include one that indicates the presence of inflammation in the body (the erythrocyte sedimentation rate), a white blood cell count, and a blood test for anemia.
X rays: X rays are used to determine the degree of joint destruction. They are not useful in the early stages of RA before bone damage is evident, but they can be used later to monitor the progression of the disease.
Treatment of Rheumatoid Arthritis
Doctors use a variety of approaches to treat RA. These are used in different combinations and at different times during the course of the disease and are chosen according to the patient's individual situation. No matter what treatment the doctor and patient choose, however, the goals are the same: relieve pain, reduce inflammation, slow down or stop joint damage, and improve the person's sense of well-being and ability to function.
Rest and exercise: Both rest and exercise help in important ways. People with RA need a good balance between the two, with more rest when the disease is active and more exercise when it is not. Rest helps to reduce active joint inflammation and pain and to fight fatigue. The length of time needed for rest will vary, but in general, shorter rest breaks every now and then are more helpful than long times spent in bed. Exercise is important for maintaining healthy and strong muscles, preserving joint mobility, and maintaining flexibility. Exercise can also help people sleep well, reduce pain, maintain a positive attitude, and lose weight.
Care of joints: Some people find that using a splint for a short time around a painful joint reduces pain and swelling by supporting the joint and letting it rest. Splints are used mostly on wrists and hands, but also on ankles and feet. A doctor or a physical or occupational therapist can help a patient get a splint that fits properly. Other ways to reduce stress on joints include helpful devices like zipper pullers, and shoe horns, devices to help with getting on and off chairs, toilet seats, and beds.
Stress reduction: People with RA face emotional challenges as well as physical ones. The emotions they feel because of the disease - fear, anger, frustration - combined with any pain and physical limitations can increase their stress level. Stress may also affect the amount of pain a person feels. Regular rest periods can help, as can relaxation, distraction, or visualization exercises. Exercise programs, participation in support groups, and good communication with the health care team are other ways to reduce stress.
Healthful diet: Studies have shown that the omega-3 fatty acids in certain fish or plant seed oils may reduce RA inflammation. However, many people are not able to tolerate the large amounts of oil necessary for any benefit. Other than these, there is no scientific evidence that any specific food or nutrient helps or harms most people with RA. However, an overall nutritious diet with enough, but not an excess of, calories, protein, and calcium is important. Some people may need to be careful about drinking alcoholic beverages because of the medications they take for RA. Patients should ask their doctors for guidance on this issue.
Climate: Some people notice that their arthritis gets worse when there is a sudden change in the weather. However, there is no evidence that a specific climate can prevent or reduce the effects of RA. Moving to a new place with a different climate usually does not make a long-term difference.
Medications
Most people who have RA take medications. Some are for pain relief; others are used to reduce inflammation. Still others, called disease-modifying antirheumatic drugs, or MARDs, are used to try to slow the course of the disease.
RA therapy traditionally involved an approach in which doctors prescribed aspirin or similar drugs, rest, and physical therapy at first, and then prescribed more powerful drugs later if the disease became much worse. But recently many doctors have changed their approach, especially for patients with severe, rapidly progressing RA. This change is based on the belief that early treatment with more powerful drugs, and the use of drug combinations in place of single drugs, may be more effective ways to halt the progression of the disease and reduce or prevent joint damage.
Surgery
Several types of surgery are available to patients with severe joint damage. These procedures can help reduce pain, improve the affected joint's function and appearance, and improve the patient's ability to perform daily activities. Surgery is not for everyone, however, and the decision should be made only after careful consideration by patient and doctor.
Joint replacement: This is the most frequently performed surgery for RA, and it is done to relieve pain, improve or preserve joint function, and improve appearance. In making a decision about replacing a joint, people with RA should consider that some artificial joints function more like normal human joints than do others. Also, artificial joints are not always permanent and may eventually have to be replaced. This may be an issue for younger people.
Tendon reconstruction: RA can damage and even rupture tendons, the tissues that attach muscle to bone. This surgery, which is used most frequently on the hands, reconstructs the damaged tendon by attaching an intact tendon to it. This helps to restore some hand function, particularly if it is done early, before the tendon is completely ruptured.
Synovectomy: In this surgery, the doctor actually removes the inflamed synovial tissue. Synovectomy by itself is seldom performed now because not all of the tissue can be removed, and it eventually grows back. Synovectomy is done as part of reconstructive surgery, especially tendon reconstruction.
Routine Monitoring and Ongoing Care
Regular medical care is important to monitor the course of RA, to determine the effectiveness and any negative effects of medications, and change therapies as needed. Monitoring typically includes regular visits to the doctor. It may also include blood, urine, and other laboratory tests and x rays.
Osteoporosis prevention is one issue that patients may want to discuss with their doctors as part of their long-term, ongoing care. Osteoporosis is a condition in which bones lose calcium and become weakened and fragile. Many older women are at increased risk for osteoporosis, and their RA increases the risk further, particularly if they are taking corticosteroids such as prednisone. These patients may want to discuss with their doctors the potential benefits of calcium and vitamin D supplements, hormone replacement therapy, or other treatments for osteoporosis.
Alternative and Complementary Therapies
Special diets, vitamin supplements, and other alternative approaches have been suggested for the treatment of RA. Although many of these approaches may not be harmful in and of themselves, controlled scientific studies either have not been conducted or have found no definite benefit to these therapies. Some alternative or complementary approaches may help reduce some of the stress associated with living with a chronic illness. As with any therapy, patients should discuss the benefits and drawbacks with their doctors before beginning an alternative or new type of therapy. If the doctor feels the approach has value and will not be harmful, it can be incorporated into a patient's treatment plan. The Arthritis Foundation (800-283-7800) publishes material on alternative therapies as well as established therapies.
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #6 on: September 29, 2006, 09:17:33 am » |
|
Better Conventional Therapy Reduces Need for Biologics for Resistant Rhuematoid Arthritis Patients
NEW ORLEANS, LA -- October 29, 2002 -- Intensified management of patients with severe rheumatoid arthritis (RA) using conventional therapy can delay or avoid the need for new biologic agents such as etanercept or infliximab.
In a British study reported here October 28 at the 66th Annual Scientific Meeting of the American College of Rheumatology, 57 percent of patients who qualified for biologics on their first clinic visit could be managed successfully for at least one additional year by more aggressive application of conventional therapies.
Lead author Sarah Bingham, MA, MRCP, research fellow at Leeds University, in Leeds, England, said her clinic for treatment-resistant patients set up a protocol to optimise therapy for the large number of patients referred for treatment with biologic agents.
She said the British Society of Rheumatology guidelines allow use of biologic agents if a patient has failed 20 mg/week of methotrexate and one other disease modifying anti-rheumatoid drug (DMARD) and still has active disease. In her hospital, the rheumatologists go beyond the guidelines, escalating conventional treatments and assessing disease activity, disability, and quality of life 12 weeks after each treatment change. If outcomes are then unacceptable, treatment is changed.
The protocol starts with monotherapy with sulphasalazine; moves to triple therapy with sulphasalazine, methotrexate, and hydroxychloroquine; then to intramuscular methotrexate; and finally to leflunomide with or without methotrexate. "And then they would go on biologics if they failed those," Dr. Bingham said.
One-year follow-up data are available on 353 patients (mean age 53 years, 71 percent female, 68 percent rheumatoid factor positive, mean disease duration of 11 years). The mean number of previously failed DMARDs was five. By 12 months, 55 percent of patients were on escalated doses of conventional therapies, and 45 percent were on biologic agents.
At study entry, 77 percent of patients had qualified for biologics based on British Society of Rheumatology criteria. Of this group, only 43 percent received biologics by one year. The rest did well with aggressive conventional therapy. This group - 57 percent of the patients who originally qualified for biologics - delayed their need for them by at least one year. Disease activity, quality of life, and disability all improved significantly for patients on conventional DMARDs (p<0.03 at 12 and 24 weeks).
The University of Leeds may be ahead of other hospitals in working out such a protocol because co-author Dr. Paul Emery had earlier access to etanercept and infliximab as a clinical investigator, and therefore, was faced with the problem of triaging patients before other medical centers. www.LupusMCTD.com
|
|
|
|
« Last Edit: January 29, 2007, 09:36:24 am by ♥Admin♥ »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #7 on: October 05, 2006, 08:34:30 am » |
|
Osteoporosis
What is it?
Osteoporosis, also called the "silent disease," is a common bone disease in which bones become thinner and more porous. Osteoporosis affects both men and women and occurs when the body fails to form new bone.
During the course of your life, the body needs the minerals phosphate and calcium to build bones. If your dietary intake of these minerals is not sufficient or if the body does not absorb enough of the minerals from the diet, bone production and bone tissue will suffer resulting in brittle and fragile bones. These bones are then subject to fracture.
You may have heard of osteoporosis referred to as the "silent disease" because it's a disease that occurs over the course of may years. The loss of bone mass does not occur overnight. It usually occurs gradually over an extended period of time. In fact, most people are not even aware that they have osteoporosis until they fracture a bone. And it's at that time that a person finds the disease is in its advance stages
What are its symptoms?
Unfortunately, there are no symptoms associated with early signs of osteoporosis. Symptoms occurring late in the disease include:
Fractures of the vertebrae, wrists or hips
Low back pain
Neck pain
Bone pain or tenderness
Loss of height over time
Stooped posture
What are the causes of osteoporosis?
Loss of estrogen due to menopause
Hormonal disorder such as Cushing's syndrome, hyperthyroidism and hyperparathyroidism
Diet low in calcium
Family history of the disease
Chronic liver disease and intestinal disorders
How is osteoporosis diagnosed?
A bone density test is used to diagnose osteoporosis. A bone density test measures bone mineral content and the strength of the bones. A low bone density test result can indicate that you may be at risk for future bone fractures. The test can also show the rate of bone mineral loss and bone gain for those receiving treatment.
How you can prevent osteoporosis
Eat a diet throughout life containing calcium, phosphorus and vitamin D. By the late 20s and into the early 30s peak bone mass is reached. You may want to talk to your doctor about taking calcium supplements when you reach this age bracket. Regular life-long exercise can also reduce the likelihood of bone fractures and weight-bearing exercise helps reduce bone mineral loss. Exercise such as walking, jogging, swimming, and skiing are all excellent for the bones, although they are not weight-bearing. Make sure you see your internist for general physical exams regularly and talk with him or her about your risk for osteoporosis and the need for a bone density test.
Is it treatable?
Yes. Although there is no cure for osteoporosis, it is a treatable disease. Many medications slow and sometimes stop bone mineral loss. Talk to your internist about proper treatment. www.LupusMCTD.com
|
|
|
|
« Last Edit: January 29, 2007, 09:23:04 am by ♥Admin♥ »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #8 on: November 16, 2006, 08:23:01 am » |
|
Treat Rheumatoid Arthritis Early
Nov. 13, 2006 (Washington) -- Two studies suggest that treating rheumatoid arthritis (RA) early and aggressively may change its course.
The findings were presented at the 2006 annual meeting of the American College of Rheumatology.
Rheumatoid arthritis is an autoimmune disease caused by the immune system attacking the lining of the joints. It can lead to long-term joint and bone damage and affects 2.1 million Americans, mainly women.
The disease can result in chronic pain, loss of function, and disability, according to the Arthritis Foundation.
There is no cure for the disease. Treatments are aimed at reducing joint inflammation and restoring joint function to near-normal levels.
Early Evidence of Rheumatoid Arthritis
In one study, Dutch researchers studied people with early evidence of rheumatoid arthritis. The researchers show that treating these individuals with the drug methotrexate can possibly prevent the disease from progressing to rheumatoid arthritis.
And in a second study, investigators report that early treatment with methotrexate plus Remicade may result in a drug-free remission in people with rheumatoid arthritis. Remicade is one of a newer category of medications that target specific chemicals that lead to inflammation.
The first study -- called PROMPT -- comprised 110 people with arthritis from an early arthritis clinic in the Netherlands. They received methotrexate or a placebo for one year. Researchers measured joint damage every six months by taking X-rays of the hands and feet -- the joints most commonly affected by rheumatoid arthritis.
People who received methotrexate showed less X-ray damage to the joints after 30 months compared with their counterparts who received a placebo. They were also less likely to develop rheumatoid arthritis, but only if they tested positive for an antibody known as anti-CCP. Anti-CCP antibodies are blood markers that may predict the development of rheumatoid arthritis.
Role of 'Personalized' Medicine
These findings point to a role for personalized medicine, says researcher Tom W.J. Huizinga, MD, chairman of rheumatology at Leiden University Medical Center in the Netherlands. "If you have autoantibodies to anti-CCP and are treated with methotrexate, you don't develop RA," he says.
"The bottom line is that patients should be referred to a rheumatologist early and if they are CCP positive, they should be treated," he says.
Steven B. Abramson, MD, the director of rheumatology at New York University and the Hospital for Joint Diseases in New York City, agrees. "This is a very exciting article [and] it clearly needs to be validated," he says. "This is the beginning of personalized medicine.
"Patients today should want to know if they are CCP positive and if they are, they should make sure their doctors treat them if they have any symptoms," he says.
Early Treatment
The second study, dubbed the BeSt study, involved a three-year follow-up that compared four of the most widely used treatments for early rheumatoid arthritis.
After two years, 55% of people treated with methotrexate plus Remicade were able to stop Remicade without relapsing and then taper off of methotrexate. By the third year, a substantial number of patients who had stopped taking Remicade were able to stop taking methotrexate and remained disease-free.
"We are very excited because this very new approach to disease hit them very early and hit them very hard with a combination of drugs," leading to remission and discontinuation of the drugs, says researcher Cornelia F. Allaart, MD, a rheumatologist at Leiden University Medical Center in Leiden, Netherlands.
Caution Urged
"These were highly selected study populations from small, highly selected study centers," cautions Iain B. McInnes, FRCP, PhD, professor of experimental medicine and rheumatology at the University of Glasgow in Scotland. "We need a whole lot more data before we can apply this to our practice," he tells WebMD. "It looks like there is a window of opportunity early in disease, but how we best target it, when we should start treatment, what drugs we should use -- and on who -- is not yet known."www.LupusMCTD.com
|
|
|
|
« Last Edit: January 29, 2007, 08:41:36 am by ♥Admin♥ »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #9 on: November 24, 2006, 08:51:31 am » |
|
Univ Develop Oral Rheumatoid Arthritis Treatments
Nov. 24, 2006
TOKYO (Nikkei)--Mitsubishi Pharma Corp. and Tokyo Medical & Dental University have separately developed candidate materials for oral medicines that are expected to be as effective as biological agents in treating rheumatoid arthritis, it has been learned.
Both groups have already confirmed the effectiveness of their respective substances through animal tests.
Mitsubishi Pharma selected the Y-320 substance from among the more than 200 types of chemical compounds it has synthesized to date. The substance was found to prevent the production of a protein seen as contributing to the inflammation of joints, one of the manifestations of rheumatoid arthritis.
A test by the Mitsubishi Chemical Holdings Corp. (4188) subsidiary showed that long-tailed macaques with rheumatoid arthritis began showing improvements after receiving daily oral doses of the substance for four weeks.
Another experiment showed that the substance had the same effectiveness as a biological agent administered via an intravenous drip or injection, and that the oral medication did not compromise the monkeys' immunity to disease like the biological agent did.
Mitsubishi Pharma hopes to commercialize the substance in several years after ensuring its long-term safety though animal testing and clinical trials on humans.
Separately, a group of researchers led by Nobuyuki Miyasaka, a professor at the medical and dental university, discovered that a substance developed for possible use in cancer drugs is effective in treating rheumatoid arthritis. The researchers found that the substance worked to suppress inflammation in the joints of mice.
Approximately 700,000 Japanese suffer from rheumatoid arthritis, particularly middle-aged and elderly women. Prolonged cases of inflammation will eventually cause joints to lose movement and become deformed.
www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #10 on: November 29, 2006, 08:16:33 am » |
|
Common Forms Of Arthritis
1)Osteoarthritis
2)Rheumatoid Arthritis
3)Gout
4)Lupus
Arthritis affects, in one form or another, 70 million Americans. Although there are more than 100 forms of arthritic conditions, four of the most common disorders include osteoarthritis, rheumatoid arthritis, systemic lupus erythematosus and gout. Arthritis may affect people of all ages, including children; the juvenile forms of arthritis are unique in how they affect the body and in how they must be treated.
1)Osteoarthritis
Among the many forms of arthritis, osteoarthritis, a degenerative joint disease (often described as a "wear and tear process"), is the most common. Osteoarthritis centers primarily on the weight-bearing joints the hip or knee, but it often affects the hand and spine as well. It occurs when the cartilage that normally covers and cushions the ends of bones wears down. As bone rubs against bone, the joint loses shape and alignment, the ends of the bones thicken and form bony growths called spurs, and bits of cartilage or bone may float within the joint space. The result is stiff, achy and sometimes swollen joints that are worse after sitting still or with use. It is estimated that almost 18 million Americans suffer from some type of degenerative joint disease.
2)Rheumatoid Arthritis
Rheumatoid arthritis affects approximately 2 million Americans. Rheumatoid arthritis is thought to be an autoimmune disease, in which the body's immune system reacts against itself causing inflammation of the lining of the joints (synovial membrane).
As the thickened and inflamed membrane spreads to the bone and cartilage, it causes swelling. In addition, enzymes are released that over time may damage bone, cartilage and ligament. The space between the joints diminishes, and the joints themselves lose shape and alignment. This chronic inflammation restricts movement and causes considerable pain, stiffness, warmth, redness and swelling at the joints.
Among the most disabling forms of arthritis, rheumatoid arthritis can result in deformed and loose joints, loss of mobility and diminished strength. Unlike other arthritic conditions that are confined to joints, rheumatoid arthritis may affect more than one joint at a time and may cause inflammation in such organs as eyes, lungs and heart. It can also produce small painless lumps under the skin, called rheumatoid nodules.
The course of the disease varies; for many it comes and goes. Some people experience symptoms continuously for a number of years. For others, the symptoms go into remission for years. Even in remission, though, there may be limited joint function as well as joint deformities.
3)Gout
Gout occurs when there is excess uric acid, one of the body's waste products, causing crystals to accumulate around the small joints. Although gout most often affects the big (or first) toe, other joints, including the ankle, foot, knee, hand and wrist, are frequently subject to gout pain and swelling.
Often episodic in nature, an attack of gout typically builds over a few hours. A joint that seems perfectly normal suddenly becomes explosively painful, red and swollen. The discomfort may last for days, but within a week or two, the joint will return to normal. If left untreated, though, repeated attacks of gout or deposits of uric acid crystals (called tophi) can result in permanent damage and disfigurement to the joint. In most cases, however, these severe forms of gout are preventable with medication. In addition, kidney stones can develop as a result as uric acid deposits. Gout affects nearly 6 million Americans of all ages, but particularly men older than 40.
4)Systemic Lupus Erythematosus, Or Lupus
Lupus is a rare, chronic connective tissue disorder that typically affects women between the ages of 15 and 35. The most common of several conditions known collectively as connective tissue or autoimmune diseases, lupus affects the lining (synovial membrane) of the joints, causing inflammation, pain and, over time, damage to the joints and connective tissue.
Symptoms of lupus include achy, swollen joints, but lupus may also affect other parts of the body. Other common problems include fever, fatigue, inflammation of the lining of the lungs and heart, anemia, skin rashes such as a butterfly-shaped rash across the cheeks and nose, sun or light sensitivity, hair loss, Raynaud's phenomenon (fingers turning white and/or blue in the cold), seizures, and mouth or nose ulcers, kidney disease or neurologic problems. Typically symptoms flare up and then subside.
Unless controlled with medications or other treatments, severe forms of lupus may affect the entire body and cause such complications as kidney failure, stroke or joint damage. For many people, lupus is a mild disease affecting only a few organs. For others, it leads to serious, even life-threatening problems.www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #11 on: November 30, 2006, 10:05:53 am » |
|
For RA Cardioprotection, Biologics Found Equal to Methotrexate
November 29, 206
BOSTON, Nov. 29 -- The biologic agents used to treat rheumatoid arthritis are no better or worse for the heart than methotrexate, according to a case-control study. Action Points
Explain to interested patients that rheumatoid arthritis causes systemic inflammation that is thought to cause the increased cardiovascular risk seen with the disease.
Caution interested patients that the results may have been biased by disease severity, which was not completely reported for patients on the various medications.
Compared with methotrexate, biologics for RA conferred no more or less risk of cardiovascular events, although oral glucocorticoid monotherapy increased the odds by 50% and other cytotoxic agents raised the risk by 80%, said Daniel H. Solomon, M.D., M.P.H., of Brigham and Women's Hospital here, and colleagues.
Their study, reported in the December issue of Arthritis & Rheumatism, compared stroke and heart attack rates in 3,501 primarily frail older patients, enrolled in a state prescription drug assistance program and Medicare, who were taking RA drugs.
Biologic agents Humira (adalimumab), Enbrel (etanercept), Remicade (infliximab) and Kineret (anakinra) as a group carried the same risk as methotrexate (odds ratio 1.0, 95% confidence interval 0.5 to 1.9), which was not significantly changed by combination with methotrexate (OR 0.8, 95% CI 0.3 to 2.0) or with other immunosuppressive agents (OR 1.2, 95% CI 0.7 to 2.2).
Oral glucocorticoid monotherapy significantly increased cardiovascular event risk compared with methotrexate (OR 1.5, 95% CI 1.1 to 2.1), with a similar trend when combined with other drugs (OR 1.3, 95% CI 0.8 to 2.0).
The cytotoxic immunosuppressive agents azathioprine, cyclosporine, and Arava (leflunomide) increased cardiovascular event risk the most of any group of agents whether as monotherapy or in combination treatment (both OR 1.8, 95% CI 1.1 to 3.0).
The noncytotoxic agents, which included gold, Plaquenil (hydroxychloroquine) and Azulfidine (sulfasalazine), did not significantly increase cardiovascular event risk compared with methotrexate (OR 1.2, 95% CI 0.8 to 1.7).
Previous studies have identified cardiovascular benefits for various agents in reducing event rates, surrogate measures and even death, but an investigation of all available immunosuppressive agents across a broad spectrum of patients with RA was lacking.
So, the researchers examined cardiovascular risk for the medications compared to methotrexate. Using RA patients not on immunosuppressive agents as the reference group would not have been appropriate, the authors wrote, because those patients may have disease remission, mild disease, or no actual RA.
The study included patients with a RA diagnosis on at least two office visits and a filled immunosuppressive medication prescription within three months. Among these were 946 cases who had been hospitalized for a cardiovascular event (438 for myocardial infarction, 639 for stroke) during the approximately two-year follow-up period.
The researchers compared each of the cases with 10 age- and sex-matched controls with RA who had not had a cardiovascular event by the time of the patient's index event.
Both groups were predominantly white (93% to 94%) and female (89% to 92%). Rheumatologic care was similar between groups though cases were more likely to have been hospitalized in the year prior to their RA diagnosis (37% versus 31%) and, as might be expected, had more cardiovascular comorbidities and medications than the control group.
In the prescription assistance program, patients received all medications for a copay of $6 without restrictions on the use of immunosuppressive agents. Each medication treatment category was mutually exclusive such that "other cytotoxic agents" included monotherapy and combination therapy but not combinations with methotrexate, biologics or glucocorticoids.
When the investigators analyzed the event rates for myocardial infarction and stroke separately, the results were similar to those of the composite findings but with widely overlapping confidence intervals. Analyses looking at glucocorticoids according to average daily dosage and cumulative dosage revealed no gradient of cardiovascular risk.
The study was limited by lack of data on important cardiovascular risk factors such as smoking and Framingham risk score and out-of-hospital events.
Also, there were no data on underlying RA severity. If patients with more severe disease who were more likely to develop cardiovascular events preferentially were channeled to the more potent methotrexate and biologic agents, there may have been a false bias against these medications.
"When studying the cardiovascular effects of an immunosuppressive agent," Dr. Solomon and colleagues wrote, "it is difficult to disentangle the effects of the medications from the underlying [RA] and its severity."
They noted that the increased cardiovascular risk found for the cytotoxic agents other than methotrexate may have been due to drug-induced hypertension, but may also reflect suboptimal control of inflammation by these agents compared to methotrexate.
Randomized, controlled studies should be done to better understand the effects of immunosuppressive agents on cardiovascular outcomes among patients with rheumatoid arthritis, the investigators concluded.
The study was supported by the Engalitcheff Arthritis Outcomes Initiative. Other relevant grant support was provided by the Arthritis Foundation, NIH, Merck, Pfizer, and Savient.
Michael, E. Weinblatt, M.D., a co-author, reported receiving consulting fees from Abbott (more than $10,000) and from Amgen, Wyeth, Centocor, Bristol-Myers Squibb, VCB, Genentech, and Roche (less than $10,000 each).
www.LupusMCTD.com |
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #12 on: December 12, 2006, 01:18:37 pm » |
|
Nutrition and Rheumatoid Arthritis
Introduction
It is estimated that collective spending by arthritis patients experimenting with unproven treatments, including diets, exceeds well over one million dollars annually. In 1989, Arthritis Care(ref 1) noted that greater than 50% of the Arthritis Care members who were surveyed, had invested in "unorthodox medicines, substances, or treatments (including diets), during the prior six months".
Since the 1930's researchers have been exploring the link between diet and arthritis. We continue to hear claims that special diets, foods and supplements may help to cure or alleviate symptoms of arthritis, but most claims are unproven. Many experts speculate that claims of nutritional remedies and cures with food or dietary supplements are related to the "placebo affect". The placebo effect is the patients perception of improved symptoms and well being, resulting from new therapy, regardless of evidence for actual physical improvement.
Because there is little scientific evidence confirming the benefits of modified diets for patients with arthritis, health care providers are apprehensive to recommend these types of dietary manipulations to their patients. Unfortunately, people with limited or no medical backgrounds have filled this void by advising patients about the benefits of diets and arthritis. The advice given is often questionable, expensive and can be dangerous.
Due to the lack of controlled studies and clinical trials, many investigators feel that we are still no closer to knowing whether food components cause or cure arthritis than we were seventy years ago. In reviewing the literature it becomes clear that there are few objective studies that examine the benefits of dietary manipulation and arthritis. This discussion will focus on diet and Rheumatoid Arthritis (RA) only since most of the available medical literature has focused on this type of arthritis.
A Healthy Diet
Until we have access to more conclusive data regarding the benefits of dietary manipulation and RA, patients are encouraged to follow a healthy, balanced diet that fosters a healthy weight. It is important to avoid elimination diets and fad nutritional practices and to be cautious of claims of miracle cures.
The fourth edition of Nutrition and Your Health: Dietary Guidelines for Americans(ref 2) outlines some basic dietary advice for all healthy Americans ages 2 years and above about food choices that promote health and prevent disease. The main messages are as follows:
Eat a variety of foods
Balance the food you eat with physical activity, maintain or improve your weight
Choose a diet with plenty of grain products and vegetables, and fruits
Choose a diet low in fat, saturated fat and cholesterol
Choose a diet moderate in sugars
If you drink alcoholic beverages, do so in moderation
Malnutrition
Patients with RA are considered to be at nutritional risk for many reasons. One cause of poor nutritional status in this patient population is thought to be the result of the weight loss and cachexia linked to cytokine production.(ref 3) In patients experiencing chronic inflammation, the production of cytokines, such as interleukin-1 and tumor necrosis factor, increases resting metabolic rate and protein breakdown. The patient then is faced with the challenge of increasing both calorie and protein intake to meet the nutritional requirements of the increased metabolic rate. This is frequently difficult secondary to the pain and swelling associated with RA which frequently make food preparation and purchasing difficult for those who live alone or have limited resources.
The effects of arthritis medications that are frequently taken long-term may also compound these nutritional problems. One example of this is observed in patients receiving methotrexate, where patients are frequently identified with folic acid deficiency. Additionally, prolonged dosing of other RA medications may be associated with conditions such as gastritis or peptic ulcer, frequently reducing a persons desire to eat.
The most commonly observed vitamin and mineral deficiencies in patients with RA, are folic acid, vitamin C, vitamin D, vitamin B6, vitamin B12, vitamin E, folic acid, calcium, magnesium, zinc and selenium.(ref 4) Although, food is always the preferred source for vitamins and minerals, it may be essential to use supplementation to assist in counterbalancing the outlined deficiencies and improving nutritional status for patients with RA. Increased intake of antioxidants such as selenium and vitamin E may decrease free-radical damage to joint linings, which diminish swelling and pain.
However, to date, there have been no human clinical trials that convincingly prove or disprove the efficacy of antioxidant use. Supplementation of calcium and vitamin D is also recommended to decrease the risk of osteoporosis that results from nutritional loss of these supplements, from menopause and from concurrent steroid therapy.
Food Hypersensitivities and Their Link to RA
In some patients, specific foods have been shown to exacerbate the symptoms of RA.(ref 5) Avoiding these foods or food groups has been shown to have limited, short term benefits but no benefits long term. Even though different forms of dietary modification have reportedly improved symptoms in some patients, people with RA may have spontaneous temporary remissions. Therefore, it is important to perform double-blind, placebo controlled trials to differentiate diet effect from spontaneous remission.
Diet elimination therapy is a method of determining food hypersensitivities with patients. Elimination diets avoid a specific food or group of foods such as milk, meat or processed foods that are known to be prime allergy suspects. These foods are eliminated from the diet for a specific period of time. Foods are then gradually reintroduced one at a time, to determine whether any of them causes a reaction.
Panush and colleagues, demonstrated temporary improvement in the signs and symptoms of RA with diet elimination and modification in a controlled study where the symptoms associated with food sensitivities were studied.(ref 5) During this study when the patient was fasting or on a severely restricted diet, the patients symptoms improved significantly. However, when the patient had milk reintroduced into the diet, episodes of pain, swollen and tender joints and stiffness were experienced. Similarly, Kjeldsen-Kragh and colleagues(ref 6) noted that fasting may be effective in reducing the symptoms of rheumatoid arthritis, however most patients relapsed as new foods were reintroduced into the diet. Pain and discomfort frequently returned once a patient reverted to a normal diet. These studies are few in number and should be interpreted and extrapolated to real life only with careful thought and caution.
Is Fasting Effective for Treating symptoms of RA?
Fasting is a very high risk, short term treatment and is currently not an accepted modality for the treatment of RA. Only a limited number of studies have shown fasting to transiently reduce joint pain in RA, and there have been no studies that have shown persistence of the improvement for greater than ten days. A general improvement in arthritic pain and swelling has been observed on day four or five of the fast, and pain and swelling generally remains absent for the duration of the fast. However, patients do not observe long term benefits from fasting and symptoms return within one week of resuming a normal diet.
Are There Benefits of Fish Oils on Arthritic Pain?
In recent years, researchers have become increasingly interested in the benefits of dietary fatty acids and their ability to modulate the inflammatory process. Dietary fatty acids such as Omega-3 fatty acids found in oils of fish and sea animals are of particular interest. Unfortunately, there have been few experiments with fish oils in patients with RA that have shown favorable results and consequently practical and safe doses are still unknown for this dietary therapy.
In most of the studies using fish oils, benefits are not usually observed until at least twelve weeks of continuous use and appear to increase with extended treatment time. It is important to note that fish oil supplements may interfere with blood clotting and increase the risk for stroke especially when consumed in conjunction with aspirin or other nonsteroidal anti-inflammatory drugs. Taking fish oils has also been linked to changes in bowel habits such as diarrhea and may also cause an upset stomach. Until more is known about safe dosing for Omega-3 fatty acids, supplementation in the form of gelatin capsules is not advised in this patient population. Rather increased consumption of fish rich in Omega 3 fatty acids such as salmon, herring and mackerel may be safer. Whether omega 3-fatty acids should be included as standard therapy for RA remains controversial.
Conclusion
In conclusion, there continues to be a great deal of discussion as to whether foods ameliorate or perpetuate arthritis, or have any effect at all. We know that in some instances, available data have been interpreted to show that there may be an association between foods and joint pain for patients with rheumatoid arthritis.
However, until more concrete, conclusive data are available to ascertain the relationship between food and rheumatic diseases, it is important to avoid unproven or unorthodox nutritional practices. Patients are encouraged to discuss diet therapy with their health care provider, follow the recommendations of the US Dietary Guidelines for Healthy Americans and add a multiple vitamin-mineral supplement that contains 100% of the Recommended Daily Intake to their diet
www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #13 on: December 15, 2006, 09:02:51 am » |
|
Mayo Clinic Foundation for Education and Research The Human Knee
ROCHESTER, MN -- December 15, 2006 --New findings from a study led by a Mayo Clinic rheumatologist indicate that men with knee osteoarthritis who smoke experience greater cartilage loss and more severe pain than men who do not smoke. Results will be published online this week in the Annals of the Rheumatic Diseases.
Knee osteoarthritis is one of the leading causes of disability in elders.
"This is a novel finding," says Shreyasee Amin, MD, Mayo Clinic rheumatologist and lead study researcher. "Previous studies showed no association between cigarette smoking and knee osteoarthritis or even a protective effect of smoking."
The finding that cigarette smoking plays a role in the worsening of knee osteoarthritis is important, says Dr. Amin, as it is a potentially modifiable risk factor.
To conduct this study, the researchers examined 159 men with symptomatic knee osteoarthritis who participated in a prospective study on the natural history of the condition, the Boston Osteoarthritis of the Knee Study.
The current study focused on men, as there were too few women in the original group studied who smoked (4%). The researchers took MRIs (magnetic resonance images) of the more symptomatic knee of each patient at the study beginning, and also 15 and 30 months later.
Cartilage loss over follow-up, based on knee MRIs, was determined at the tibiofemoral joint (the connection between the thighbone and shinbone) and the patellofemoral joint (the junction of the knee cap and the thigh bone) in the knees, and a scoring tool was used to assess knee pain severity.
Nineteen, or 12%, of the men were current smokers at the study's start. These men also were leaner and younger than other study participants, so the researchers adjusted for these factors. The investigators found current smokers had a 2.3 fold increased risk of cartilage loss at the medial tibiofemoral joint and a 2.5 fold increased risk of cartilage loss at the patellofemoral joint compared to the men who had quit smoking or never smoked. Current smokers also had higher pain scores than men who were not current smokers, at the beginning of the study (60.5 vs. 45.0, with 100 as the highest possible pain score) and at follow up (59.4 vs. 44.3).
The association between smoking and cartilage loss in knee osteoarthritis could be explained by one or more of the following theories, according to the researchers:
*Smoking may disorder the cells and inhibit cell proliferation in the knee cartilage
*Smoking may increase oxidant stress, which contributes to cartilage loss
*Smoking may raise carbon monoxide levels in arterial blood, contributing to tissue hypoxia (insufficient blood oxygenation), which could impair cartilage repair
Dr. Amin and colleagues believe that the increased pain experienced by smokers with knee osteoarthritis may not be due to the effect of smoking on cartilage loss, as cartilage does not have pain fibers. They have several theories for the link:
*Smoking may affect other knee joint structures mediating knee pain
*Smoking may affect one's pain threshold for knee or other musculoskeletal pain
Dr. Amin says these findings are provocative and deserve further study, especially given the number of potential ways in which cigarette smoking could have a negative effect on knee joint cartilage.
Osteoarthritis, sometimes called degenerative joint disease or osteoarthrosis, is the most common form of arthritis. Osteoarthritis is characterized by the breakdown of joint cartilage and may affect any bodily joint, including those in the fingers, hips, knees, lower back and feet, though weight-bearing joints such as the knees are most susceptible. As cartilage slowly deteriorates over the years, chronic pain or varying amounts of discomfort can arise when standing and walking, and swelling also may occur with knee osteoarthritis. Over time, the cartilage deteriorates, and its smooth surface roughens. Eventually, if the cartilage wears down completely, bone may rub on bone, causing the ends of the bones to become damaged and the joints to become more painful. There is no known cause or cure for osteoarthritis, but available treatments can relieve pain and help patients remain active.
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #14 on: December 18, 2006, 05:04:58 pm » |
|
FDA Expands Celebrex Use for Juvenile RA
The Food and Drug Administration has approved the marketing of the painkiller Celebrex as a treatment for children 2 and older with juvenile rheumatoid arthritis. The drug is already used off-label by some physicians as a treatment for the disease, which affects up to 60,000 children. The FDA said it would require the manufacturer to continue studying the safety of the medication in children, especially its long-term effects on the kidneys, blood pressure, and heart. www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #15 on: December 19, 2006, 12:32:28 pm » |
|
**NOTE~I posted this last year and feel it's worth reposting again this year. How to Reduce Holiday Arthritis Flares
Tips on Controlling Your Arthritis
Many people with inflammatory types of arthritis, such as rheumatoid and lupus, report that their illness flares during and after the holidays. That should be no surprise because holidays can be stressful - and physical and emotional stress can increase the risk of flares.
Pace Yourself - If you're hosting the family get-together or throwing a party for friends, pace yourself. Start planning weeks ahead. Write down your plans, and set priorities - dates when you will do specific shopping, times when you will do advance cooking. Then relax - and build rest-times into your schedule. If you pace yourself and have lists so you know what you need to do when, you will be better able to get through.
Get Help - Don't be a martyr. Delegate tasks and ask for help. Those who love you will welcome an opportunity to help you - and to be an important part of the event. If you do it all yourself, you may find resentment building up - which will ruin your enjoyment of the party.
Set Aside Time for Yourself - Block out some solitary periods on your winter social calendar. You need time to recharge your batteries. All those candles should not be for parties. Light some for yourself to give you a light in the darkness - a place on which to focus for relaxation, meditation, or prayer - all great ways to recharge your batteries. Or light a candle in the bathroom while you relax in a warm tub - also great for achy joints. And don't forget your regular exercise regimen - because exercise keeps you conditioned and can replace fatigue with energy.
Don't Overspend - Set a budget, and do your best to stick to it - whether it's for party planning or gift-giving. If you overspend, worry will be your secret companion - and stressor - for months to come.
Practice Positive Self-Talk - Try to avoid worrying thoughts, such as "There's too much to do, I'll never be ready." If you've done your planning and arranged for friends and family to help, you really are ready. Think steadying thoughts, such as "Calm down and check your list, take one step at a time, and I'll be fine."
Don't Miss Your Meds - With all the holiday excitement, it's easy to miss your meds - whether that means ordering them on time or taking them on time. Put prescription order dates on your calendar. And if you don't already have one of those little boxes that keeps your pills in order by day of the week, that's a gift to get for yourself right now. Then keep it next to your toothbrush so you'll never forget - morning and evening.
If despite following this advice you start feeling signs of a flare, pay attention. Don't try denial hoping it will get better on its own. The sooner a flare is treated, the sooner it is controlled. Call your doctor promptly.
www.LupusMCTD.com |
|
|
|
« Last Edit: December 19, 2006, 07:35:45 pm by Kathy »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #16 on: December 26, 2006, 06:34:29 pm » |
|
CRP Levels Not Predictive of Rheumatoid Arthritis in Women
December 26, 2006 Although C-reactive protein (CRP) levels have been shown to correlate with rheumatoid arthritis (RA) disease activity, they are not predictive of incident RA in women, according to a report in the Archives of Internal Medicine for December 11/25.
Recognizing RA at a preclinical stage could be useful in preventing disability from the disease. Biomarkers that have shown some promise in identifying patients destined to develop this condition include rheumatoid factor and anticyclic citrullinated peptide antibodies.
Whether CRP, a marker of systemic inflammation, can predict RA is unclear. Two reports have linked elevated CRP levels with the development of RA, while another found no association between CRP levels and RA up to 20 years prior to diagnosis.
To investigate further, Dr. Nancy A. Shadick, from Brigham and Women's Hospital in Boston, and colleagues analyzed data for more than 27,000 participants in the Women's Health Study, a trial begun in 1992 to evaluate the cardiovascular effects of aspirin and vitamin E. Blood samples taken at enrollment were analyzed for CRP levels. The women were 45 years of age or older, and had no history of cardiovascular disease or cancer at randomization.
During nearly 10 years of follow-up, there were 398 self-reports of RA. Ninety of these cases were confirmed on chart review using American College of Rheumatology criteria, the authors note.
After adjusting for randomized treatment, age, BMI, and smoking, the authors found that the CRP level was not significantly associated with the development of RA. Further analysis showed that this held true regardless of the time from CRP measurement to diagnosis.
"A baseline CRP measurement is predictive of MI, stroke, and cardiovascular death," Dr. Shadick told Reuters Health. "But, CRP does not predict incident cancer and, in our study, it did not predict RA."
Dr. Shadick emphasized that CRP testing still has a place in the management of patients with established RA, as it has proven useful in gauging disease activity.
Learning Objectives for This Educational Activity
Upon completion of this activity, participants will be able to:
Identify markers of RA evident prior to the development of clinical disease.
Specify the value of CRP in predicting RA among asymptomatic women.
Clinical Context
The treatment of RA focuses on improving long-term pain and dysfunction due to disease, and earlier treatment with disease-modifying medications helps to promote this goal. To this end, researchers have examined several possible biomarkers that may predict RA in asymptomatic adults, and they have found that the presence of rheumatoid factor increases the risk of developing RA. Also, anticyclic citrullinated peptide molecules, including antikeratin antibody and antiperinuclear factor, may predict RA prior to symptoms.
While CRP levels are often elevated among patients with active RA, the usefulness of this readily available laboratory measurement in predicting RA is less clear. The authors of the current research examine data from the Women's Health Study to assess the predictive value of CRP for RA.
Study Highlights
The main research question of the Women's Health Study was the effect of aspirin and vitamin E supplementation on the risks for cardiovascular disease and cancer. All participants were female health professionals at age 45 years or older. Women with a history of cardiovascular disease or cancer at baseline were excluded from study participation.
Women completed a baseline health screening questionnaire, which was updated annually. 71% of the study cohort also provided blood samples at baseline.
The current analysis excluded patients who reported RA at baseline. Incident RA was diagnosed by self-report, and women who reported RA then completed a validated questionnaire of symptoms. Women with a positive questionnaire had the diagnosis of RA corroborated by a review of medical records.
The main study outcome was the relationship between high-sensitivity levels of CRP at baseline, which was divided into tertiles, and the development of incident RA. Results were adjusted for age, study treatment, body mass index, postmenopausal hormone use, breast-feeding, and smoking.
Data from 27,213 women were included in the current study, and the mean duration of follow-up was 10 years. 398 women reported a diagnosis of RA during this period, and 90 cases were confirmed on review of the medical record.
Women with incident RA were less likely to smoke than women without RA, but other characteristics were similar between groups.
The mean levels of CRP among women who did and did not develop RA were 3.4 and 3.6 mg/dL, respectively, a nonsignificant difference.
On multivariate analysis, the relative risks of developing record-confirmed RA associated with the first (referent), second, and third tertiles of CRP were 1.00, 0.93, and 1.18, respectively. There was no significant trend toward an increased risk for RA linked with rising levels of CRP. Also, CRP was not useful in predicting self-reported RA or RA confirmed by questionnaires of symptoms.
There was no significant interaction between when blood was drawn for CRP levels and the diagnosis of RA, indicating that CRP was not helpful as a marker of preclinical RA at any time prior to diagnosis.
Pearls for Practice
Established biomarkers that may predict the development of RA among asymptomatic adults include rheumatoid factor, antikeratin antibody, and antiperinuclear factor.
In the current study, CRP was not a significant predictor of incident RA among middle-aged women.www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #17 on: January 11, 2007, 08:21:23 am » |
|
Prevalence of Arthritis
An estimated 46 million adults in the United States reported being told by a doctor that they have some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia.
One in five (21%) adults in the United States report having doctor diagnosed arthritis.
In 2002, 51% of adults 75 years and over reported an arthritis diagnosis.
By 2030, an estimated 67 million of Americans aged 18 years or older will have doctor-diagnosed arthritis.
Hootman JM, Helmick CG. Projections of US prevalence of arthritis and associated activity limitation
Prevalence of Specific Types of Arthritis
The most common form of arthritis is osteoarthritis. Other common rheumatic conditions include gout, fibromyalgia and rheumatoid arthritis.
An estimated 21 million adults have osteoarthritis.
An estimated 2.1 million adults are affected by rheumatoid arthritis
An estimated 5.1 million adults report having a doctor diagnosis of gout.
An estimated 3.7 million adults have fibromyalgia.
Prevalence of Arthritis by Age/Race/Gender
Of persons aged 1844, 7.9% (8.5 million) report doctor-diagnosed arthritis. Of persons aged 4564, 28.8% (18.5 million) report doctor-diagnosed arthritis. Of persons aged 65+, 47.8% (15.7 million) report doctor-diagnosed arthritis.
25.9 million women and 16.8 million men report doctor-diagnosed arthritis.
2.6 million Hispanic adults report doctor-diagnosed arthritis.
4.5 million Non-Hispanic Blacks report doctor diagnosed arthrit
Overweight/Obesity and Arthritis (adult aged ≥18)
People who are overweight or obese report more doctor-diagnosed arthritis than thinner people.
15% of under/normal weight adults report doctor-diagnosed arthritis.
17.5% of people of normal weight report doctor-diagnosed arthritis.
21% of overweight and 31% among obese Americans report doctor-diagnosed arthritis.
66% of adults with doctor-diagnosed arthritis, are overweight or obese (compared with 53% of adults without doctor-diagnosed arthritis).
Weight loss of as little as 11 pounds reduces the risk of developing knee osteoarthritis by 50%.
Physical Activity and Arthritis
Almost 44% of adults with doctor-diagnosed arthritis report no leisure time physical activity; 36% of adults without arthritis report no leisure time physical activity.
Among adults with knee osteoarthritis, engaging in moderate physical activity at least 3 times per week can reduce the risk of arthritis-related disability by 47%.
Disability/Limitations and Arthritis
Arthritis and other rheumatic conditions are the leading cause of disability in the United States.
Approximately 38% (17 million) of adults with doctor-diagnosed arthritis report arthritis-attributable activity limitations; [7.8% of all US adults.].
30.6% of adults aged 18-64 with doctor-diagnosed arthritis report an arthritis-attributable work limitation.
Among adults with doctor-diagnosed arthritis, many report significant limitations in vital activities such as:
walking 1/4 mile6 million
stooping/bending/kneeling7.8 million
climbing stairs4.8 million
social activities such as church and family gatherings2.1 million
Among all civilian, non-institutionalized U.S. adults 7.8% report both doctor-diagnosed and arthritis attributable activity limitations.
Among all civilian, non-institutionalized U.S. adults aged 18-64, 4.8% (8.2 million) report both doctor diagnosed arthritis and arthritis-attributable work limitations.
www.LupusMCTD.com |
|
|
|
« Last Edit: January 11, 2007, 08:23:13 am by ♥Admin♥ »
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #18 on: January 12, 2007, 09:38:10 am » |
|
January 12, 2007
Arthritis, Rheumatism Cost U.S. $128B
ATLANTA (AP) -- The nation's costs for arthritis and related conditions rose to $128 billion in 2003, and the tab will continue to grow as the U.S. population gets older and heavier, the government said Thursday.
The 2003 costs, the latest data available, included $80.8 billion in direct costs, such as medical expenses, and $47 billion in indirect costs, such as lost wages, the Centers for Disease Control and Prevention said.
The total was a 48 percent increase over the 1997 figure of $86.2 billion cost, largely because government surveys identified 9 million more cases of arthritis or related conditions, the CDC said.
The CDC estimated that 46.1 million people were treated for arthritis and other rheumatic conditions in 2003, and 29.5 million of them lost earnings. The government estimates 8 million more people will suffer from arthritis between 2005 and 2015.
The government recommended lowering costs with widespread use of self-management programs, which teach patients how to manage their pain and continue working with the condition.
California had the largest costs from arthritis at $12.1 billion, followed by $8.7 billion in New York and Texas, and $7.6 billion in Florida.www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #19 on: January 29, 2007, 08:14:53 am » |
|
Steroids Slow Early Rheumatoid Arthritis
January 29, 2007
LIVERPOOL, England, Jan. 26 -- Low-dose glucocorticoid agents given along with standard disease-modifying drugs (DMARDs) reduced the progression of early rheumatoid arthritis for up to two years, Cochrane reviewers reported.
All the studies reviewed, except one, showed a numerical benefit in favor of the steroids, which were generally used along with DMARDs, according to a report in the January issue of the Cochrane Database of Systematic Reviews.
From an average of all the studies, the reduction of erosion progression was 60% or more when the glucocorticoids were used along with DMARDs, said John Kirwan, M.D., of Liverpool Women's Hospital here, and colleagues.
These findings were derived from a Medline search (1966 to 2005) and the Cochrane Controlled Trials Register, which produced 15 studies including 1,414 patients, older than 18.
The comparisons included either placebo or active controls (non-steroidal anti-inflammatory drugs (NSAIDS), DMARDs, but no steroids) with x-rays of hands, feet, or hands and feet. Most of the trials studied disease progression up to two years.
The daily dose of steroid was 10 mg or less of prednisone equivalent. The mean cumulative dose was 2,300 mg prednisone equivalent (range 270 mg-5,800 mg) over the first year. In most cases the drugs were added to other disease-modifying anti-rheumatoid drugs.
The standardized mean difference in progression was 0.40 in favor of steroids (95% CI 0.27-0.54), the researchers reported.
In studies of 806 patients lasting two years, the standardized mean difference in progression in favor of glucocorticoids at one year was 0.45 (CI 0.24-0.66). At two years, it was 0.42 (0.30-0.55), the researchers reported.
The proportion of benefit gained by steroids in reducing he progress of erosion from an average of all the studies over one year was 59.8% (CI, 45.4%- 74.1%), the researchers said.
Using data from trials lasting two years, the proportion of benefit gained by steroids in reducing erosion progression at one year was 67.2% (48.9%-85.4%). Over two years, it was 61.3% (46.5%-76.1%).
Furthermore, the researchers said, this benefit was achieved in patients who were for the most part receiving disease-modifying anti-rheumatoid drug treatment. It therefore represents a gain over and above any benefit from the disease-modifying drugs alone.
However, Dr. Kirwan added, the beneficial effects of glucocorticoids were generally achieved when used with the disease-modifying drugs.
Steroids were also found beneficial in an analysis of studies in which they were given along with and compared with disease-modifying anti-rheumatoid drugs plus NSAIDs. There was a significant benefit when step-down glucocorticoids taken with the disease modifiers plus NSAIDs were compared with disease modifying drugs plus NSAIDs, and in patients taking only NSAIDs, the investigators said.
The principle analysis included all studies with all types of glucocorticoid administration, even though it is possible, even likely, that the efficacy of glucocorticoids depends on the route of administration and the use of concomitant medications, the investigators said.
It should be recognized that the link between radiological benefit and overall long-term functional benefit is not firmly established, and it does not necessarily follow that patients will gain long-term functional improvement, the researchers said.
Although the potential for high doses of these drugs to cause adverse effects is well known, the doses used in many of these studies were low, they said. Nevertheless, the potential for adverse effects at low doses is less clear, they said.
Safety data from recent randomized controlled clinical trials of low dose glucocorticoid treatment in rheumatoid arthritis suggest that adverse effects associated with these drugs are modest, and often not statistically different from those of placebo.
The most immediate concern, reduced bone mineral density, can now be readily treated, they said. "Therefore, we believe the evidence that glucocorticoids given in addition to standard therapy can substantially reduce the rate of erosion progression in rheumatoid arthritis is convincing, and that the use of such treatment should be made readily available to patients," the investigators said.
It also seems likely that patients with a disease duration of three or four years might benefit, but it would be inappropriate to extrapolate into longer disease durations without more firm evidence of benefit, the researchers said.
Nevertheless, they added, there remains concern about potential long-term adverse reactions to glucocorticoid therapy, such as increased cardiovascular risk, and this issue requires further research.
-www.LupusMCTD.com-
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #20 on: February 01, 2007, 08:39:09 pm » |
|
New Score Helps Spot Rheumatoid Arthritis Sufferers
Early detection is important to safe, effective treatment, experts say
Thursday Feb.01, 2007-- Dutch researchers may have a new method of predicting whether patients with arthritic symptoms will progress to the autoimmune form of the disease, rheumatoid arthritis.
By differentiating those patients who will develop full-blown rheumatoid arthritis from those who will not, the new formula could speed earlier treatment of rheumatoid arthritis patients, reducing damage to their joints while sparing those who will not develop the disease the side effects sometimes associated with rheumatoid arthritis drugs.
"You don't want to give treatment to patients who will spontaneously remit, because they will not get the benefit," explained lead researcher Dr. Annette van der Helm-van Mil, a rheumatologist at Leiden University Medical Center in the Netherlands. "You want to give it only to the patients who have a high chance of progressing to rheumatoid arthritis."
According to the Arthritis Foundation, rheumatoid arthritis is an autoimmune disease that affects some 2.1 million Americans, most of them women. The disease often presents first as "undifferentiated arthritis," a condition that lacks the criteria for a more definitive diagnosis. Up to 50 percent of patients with undifferentiated arthritis will spontaneously go into remission, while another third will progress to rheumatoid arthritis.
The problem, said van der Helm-van Mil, is that treatment of rheumatoid arthritis with the rug methotrexate at this point can reduce future joint damage but is also potentially toxic. That's why spotting patients with true rheumatoid arthritis early is so important.
In their study, the Dutch group studied a cohort of 570 patients who presented to the Leiden Early Arthritis Clinic with undifferentiated arthritis, 177 of whom progressed to rheumatoid arthritis within one year.
They identified nine variables, including gender, age, the number and distribution of stiff and swollen joints, and three laboratory tests. When factored into an algorithm, these factors could predict the likelihood of developing rheumatoid arthritis with nearly 90 percent accuracy.
Scores from this "prediction rule" ranged from zero to 14. Patients who score six or below have a 91 percent chance of not developing rheumatoid arthritis, the researchers said, while those who score above 8 have an 84 percent chance of progressing to the autoimmune disease. Those who score seven (about 25 percent of patients) have a 50/50 chance of developing rheumatoid arthritis, while those who score above 10 have a 100 percent chance of developing the disease.
"Using information like this can be extremely helpful in managing patients," said Dr. Clifton Bingham III, assistant professor of medicine in the divisions of rheumatology and allergy and clinical immunology at the Johns Hopkins Arthritis Center in Baltimore, Md. "One of the large questions we face in patients who present with undifferentiated arthritis is knowing which of those patients should receive more aggressive therapy to minimize the long-term consequences of the disease or to decrease the likelihood of going on to develop rheumatoid arthritis," he explained.
Bingham noted, however, that this information may be more useful in the United States for primary care physicians than for rheumatologists. The formula already reflects common practice among rheumatologists, he said. Plus, health care differences between the Netherlands and the United States mean that rheumatologists in the U.S. may be less likely to see patients with undifferentiated arthritis than their counterparts in Leiden, because in the U.S., these patients are more likely to present to primary care doctors first. By the time the patient gets to a rheumatologist, he or she has often already developed more-definite rheumatoid arthritis, Bingham said.
"So, it provides a decision tool for primary care doctors to use in determining which patients are most appropriate for early referral to a rheumatologist," he said.
Bingham cautioned that several caveats must be considered before implementing this prediction score in the United States. First, it needs to be validated in other locales and with other patient populations. Second, he cautioned against using this test to produce strict cutoff values for treatment, since what might be true in a population isn't always true for an individual patient. Finally, he noted that the study doesn't address which treatment regimen is most effective once a patient actually develops rheumatoid arthritis.
"We face that question [of treatment] perhaps more often than the question being raised in this study," Bingham said. "We don't yet know how to answer that question."
The methods used in this study could possibly be used to help solve that puzzle, he added.
-www.LupusMCTD.com-
[/color] |
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #21 on: March 02, 2007, 11:01:54 am » |
|
Remicade Receives Approval in European Union for Dosing Flexibility in the Treatment of Rheumatoid Arthritis
Mar. 02, 2007
Revised Labeling Will Allow RA Patients to Receive Adjusted Dosage To Maximize Efficacy and Symptom Relief
For patients who had an incomplete response to initial combination treatment with methotrexate and REMICADE 3 mg/kg, the dose titration label extension will permit physicians to increase the REMICADE dose stepwise from 3 mg/kg up to 7.5 mg/kg every 8 weeks, or to treat patients with 3 mg/kg as often as every 4 weeks.
"Offering physicians the option to adjust dosing is welcome news for European rheumatologists who regularly manage rheumatoid arthritis patients," said Iain B. McInnes, FRCP, PhD, Professor of Experimental Medicine, University of Glasgow, Honorary Consultant Rheumatologist, Centre for Rheumatic Diseases, Glasgow Royal Infirmary, Glasgow, United Kingdom.
"The European Commission approval of the dose titration label extension will allow physicians greater flexibility to adjust the dose of REMICADE to ensure rheumatoid arthritis patients are getting optimal treatment," said Robert J. Spiegel, MD, chief medical officer, Schering-Plough Research Institute. "This latest regulatory milestone further validates the safety and efficacy profile of REMICADE for the treatment of patients with rheumatoid arthritis."
The EC approval for the dose titration label extension is based on data from the Safety Trial for Rheumatoid Arthritis with REMICADE (infliximab) Therapy (START), a randomized, multi-center, double-blind, three-arm, parallel-group, placebo-controlled study involving 1,082 treated patients with active RA. In one study arm beginning at week 22 (group 2, n=329), eligible patients that met predefined criteria for lack of response or loss of response were allowed to dose titrate with 1.5 mg/kg increments from 3 mg/kg up to 9 mg/kg. The majority (67 percent) of these patients did not require any dose titration. Of the patients who required a dose titration, 80 percent achieved clinical response and the majority (64 percent) of these required only one adjustment of 1.5 mg/kg.
~About Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a chronic, debilitating inflammatory disease that causes pain, swelling, stiffness, and loss of function in the joints. Symptoms of RA include inflammation of the joints, swelling, difficulty moving, and pain. The most commonly affected joints are the hands and feet. The joint pain of RA can impact a patient's ability to perform normal daily activities, limit job opportunities, and make family and household responsibilities a challenge. RA afflicts more than 9.7 million people worldwide; according to the World Health Organization, the incidence of RA in Europe is expected to increase over the next decade as the population ages.
~About START
The START study was undertaken to better characterize the safety profile of REMICADE plus methotrexate in combination with background treatments during one year in a population of RA patients who may have existing comorbidities. The primary objective of this study was to assess the relative risk of serious infections within the first 22 weeks after treatment with REMICADE in combination with methotrexate, in RA patients that had demographics reflective of patients seen in clinical practice. In addition, the study evaluated the effect of escalating doses in those patients who exhibited an incomplete response to the lowest approved dose, 3 mg/kg given every 8 weeks.
In START, patients with active RA despite receiving MTX were randomly assigned to receive infusions of placebo (group 1, n _ 363), REMICADE 3 mg/kg (group 2, n _ 360), or REMICADE 10 mg/kg (group 3, n _ 361) at weeks 0, 2, 6, and 14. At week 22, patients in placebo group 1 began receiving REMICADE 3 mg/kg every 8 weeks, and patients in group 3 continued to receive REMICADE 10 mg/kg every 8 weeks. In group 2 (n=329), patients with an inadequate response received increasing doses of REMICADE at 1.5 mg/kg increments from 3 mg/kg up to 9 mg/kg, administered every 8 weeks. The majority (67 percent) of patients in group 2 did not require any dose titration. Of the patients who required a dose titration, 80 percent achieved clinical response and the majority (64 percent) of these required only one adjustment of 1.5 mg/kg.
Results of the START study found that the risk of serious infections in patients receiving REMICADE 3 mg/kg plus methotrexate was similar to that in patients receiving methotrexate alone. Patients receiving the unapproved induction regimen of REMICADE 10 mg/kg plus methotrexate followed by a 10 mg/kg maintenance regimen had an increased risk of serious infections through week 22. Through week 54, 1 patient in group 1, 2 patients in group 2, and 4 patients in group 3 developed active tuberculosis. During weeks 22-54, serious adverse events among subjects in group 2 that did not dose titrate versus subjects that did dose titrate were 4 percent and 6 percent, respectively; serious infections occurred in 0.5 percent and 0 percent of subjects, respectively.
~About REMICADE
REMICADE is a monoclonal antibody that specifically targets TNF-alpha, which has been shown to play a role in Crohn's disease (CD), rheumatoid arthritis (RA), ankylosing spondylitis (AS), psoriatic arthritis (PsA), ulcerative colitis (UC) and psoriasis (PsO). REMICADE is the global market leader among anti-tumor necrosis factor alpha (TNF-alpha) therapies and the only agent approved for the treatment of both RA and CD in North America, the EU and Japan. The safety and efficacy of REMICADE have been well established in clinical trials over the past 14 years and through commercial experience with nearly 840,000 patients treated worldwide.
In the EU, REMICADE is indicated for the treatment of severe, active CD in patients who have not responded despite a full and adequate course of therapy with a corticosteroid and/or an immunosuppressant; or who are intolerant to or have medical contraindications for such therapies. REMICADE also is indicated for the treatment of fistulizing, active CD in patients who have not responded despite a full and adequate course of therapy with conventional treatment (including antibiotics, drainage and immunosuppressive therapy).
For RA patients in the EU, REMICADE, in combination with methotrexate, is indicated for the reduction of signs and symptoms as well as the improvement in physical function in patients with active disease when the response to disease-modifying drugs, including methotrexate, has been inadequate, and in patients with severe, active and progressive disease not previously treated with methotrexate or other DMARDs. In these patient populations, a reduction in the rate of the progression of joint damage, as measured by X-ray, has been demonstrated.
In the EU, REMICADE is also indicated for the treatment of AS in patients who have severe axial symptoms, elevated serological markers of inflammatory activity and who have responded inadequately to conventional therapy. REMICADE is also approved for the treatment of active and progressive PsA in adults when the response to previous disease-modifying anti-rheumatic drugs therapy has been inadequate. REMICADE should be administered in combination with MTX or alone in patients who show intolerance to MTX or for whom MTX is contraindicated. REMICADE is also approved in the EU for the treatment of moderate to severe plaque psoriasis in adults who failed to respond to, or have a contraindication to, or are intolerant of other systemic therapy including cyclosporine, MTX or PUVA (psoralen plus ultraviolet A light).
In February 2006, REMICADE was approved in the EU for the treatment of moderately-to-severely active UC in patients who have had an inadequate response to conventional therapy, including corticosteroids and 6-MP or AZA, or who are intolerant to or have medical contraindications for such therapies. This approval made REMICADE the first and only biologic therapy approved to treat moderate-to-severe UC in the EU.
REMICADE is the only anti-TNF biologic therapy available as an IV form. Unlike self-administered therapies that require patients to inject themselves frequently, REMICADE is the only anti-TNF biologic administered directly by caregivers in the clinic or office setting. In RA (3 mg/kg), CD (5 mg/kg), PsA (5 mg/kg), psoriasis (5 mg/kg) and UC (5 mg/kg), REMICADE is a two-hour infusion administered every 8 weeks, following a standard induction regimen that requires treatment at weeks 0, 2 and 6. As a result, REMICADE patients may require as few as six treatments each year. In AS (5 mg/kg), REMICADE is a two-hour infusion administered every 6 to 8 weeks, following a standard induction regimen that requires treatment at weeks 0, 2 and 6. In carefully selected patients with RA who have tolerated three initial two-hour infusions of REMICADE, consideration may be given to administering subsequent infusions over a period of not less than one hour. Shortened infusions at doses greater than 6 mg/kg have not been studied.
Furthermore, if an RA patient has an inadequate response or loses response after initial treatment with REMICADE, consideration may be given to increase the dose step-wise by approximately 1.5 mg/kg, up to a maximum of 7.5 mg/kg every 8 weeks. Alternatively, administration of 3 mg/kg as often as every 4 weeks may be considered. If adequate response is achieved, patients should be continued on the selected dose or dose frequency. Continued therapy should be carefully reconsidered in patients who show no evidence of therapeutic benefit within the first 12 weeks of treatment or after the dose has been adjusted.
REMICADE treatment is to be initiated and supervised by qualified physicians experienced in the diagnosis and treatment of rheumatoid arthritis, inflammatory bowel diseases, ankylosing spondylitis, psoriatic arthritis or psoriasis. REMICADE infusions should be administered by qualified healthcare professionals trained to detect any infusion related issues. Patients treated with REMICADE should be given a package leaflet and a special alert card.
Centocor discovered REMICADE and has exclusive marketing rights to the product in the United States. Schering-Plough markets REMICADE in all countries outside of the United States, except in Japan and parts of the Far East where Tanabe Seiyaku, Ltd. markets the product and in China where Xian-Janssen markets REMICADE.
~Important Safety Information
There are reports of serious infections, including tuberculosis (TB), sepsis and pneumonia. Some of these infections have been fatal. Tell your doctor if you have had recent or past exposure to people with TB. Your doctor will evaluate you for TB and perform a TB test. If you have latent (inactive) TB, your doctor should begin TB treatment before you start REMICADE. REMICADE can lower your ability to fight infections, so if you are prone to or have a history of infections, or develop any signs of an infection such as fever, fatigue, cough, flu or warm, red or painful skin while taking REMICADE, tell your doctor right away. Also, tell your doctor if you are scheduled to receive a vaccine or if, you have lived in a region where histoplasmosis or coccidioidomycosis is common.
Reports of a type of blood cancer called lymphoma in patients on REMICADE or other TNF blockers are rare but occur more often than expected for people in general. People who have been treated for rheumatoid arthritis, Crohn's disease, ankylosing spondylitis, psoriatic arthritis, or plaque psoriasis for a long time, particularly those with highly active disease may be more prone to develop lymphoma. Cancers, other than lymphoma, have also been reported. Children and young adults who have been treated for Crohn's disease with REMICADE have developed a rare type of lymphoma that often results in death. These patients also were receiving drugs known as azathioprine or 6-mercaptopurine. If you take REMICADE or other TNF blockers, your risk for developing lymphoma or other cancers may increase. You should also tell your doctor if you have had or develop lymphoma or other cancers or if you have a lung disease called chronic obstructive pulmonary disease (COPD).
Many people with heart failure should not take REMICADE; so prior to treatment you should discuss any heart condition with your doctor. Tell your doctor right away if you develop new or worsening symptoms of heart failure (such as shortness of breath, swelling of your ankles or feet, or sudden weight gain.
Reactivation of hepatitis B virus has been reported in patients who are carriers of this virus and are taking TNF blockers, such as REMICADE. Some of these cases have been fatal. Tell your doctor if you know or think you may be a carrier of hepatitis B virus or if you experience signs of hepatitis B infection, such as feeling unwell, poor appetite, tiredness, fever, skin rash and/or joint pain.
There have been rare cases of serious liver injury in people taking REMICADE, some fatal. Tell your doctor if you have liver problems and contact your doctor immediately if you develop symptoms such as jaundice (yellow skin and eyes), dark brown urine, right-sided abdominal pain, fever, or severe fatigue.
Blood disorders have been reported, some fatal. Tell your doctor if you develop possible signs of blood disorders such as persistent fever, bruising, bleeding, or paleness while taking REMICADE. Nervous system disorders have also been reported. Tell your doctor if you have or have had a disease that affects the nervous system, or if you experience any numbness, weakness, tingling, visual disturbances or seizures while taking REMICADE.
Allergic reactions, some severe have been reported during or after infusions with REMICADE. Signs of an allergic reaction include hives, difficulty breathing, chest pain, high or low blood pressure, swelling of face and hands, and fever or chills. Tell you doctor if you have experienced a severe allergic reaction. The most common side effects of REMICADE are: respiratory infections, such as sinus infections and sore throat, headache, rash, coughing, and stomach pain.
For complete EU prescribing information, please visit www.emea.eu.int.
~About Centocor
Centocor is harnessing the power of world-leading research and biomanufacturing to deliver innovative biomedicines that transform patients' lives. Centocor has already brought innovation to the treatment of Crohn's disease, rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis, ulcerative colitis, pediatric Crohn's disease and psoriasis.
The world leader in monoclonal antibody production and technology, Centocor has brought critical biologic therapies to patients suffering from debilitating immune disorders. Centocor, Inc. is a wholly owned subsidiary of Johnson & Johnson.
This press release contains "forward-looking statements" as defined in the Private Securities Litigation Reform Act of 1995. These statements are based on current expectations of future events. If underlying assumptions prove inaccurate or unknown risks or uncertainties materialize, actual results could vary materially from the Company's expectations and projections. Risks and uncertainties include general industry conditions and competition; economic conditions, such as interest rate and currency exchange rate fluctuations; technological advances and patents attained by competitors; challenges inherent in new product development, including obtaining regulatory approvals; domestic and foreign health care reforms and governmental laws and regulations; and trends toward health care cost containment. A further list and description of these risks, uncertainties and other factors can be found in Exhibit 99 of the Company's Annual Report on Form 10-K for the fiscal year ended January 1, 2006. Copies of this Form 10-K, as well as subsequent filings, are available online at www.sec.gov or on request from the Company. The Company does not undertake to update any forward-looking statements as a result of new information or future events or developments.
~About Schering-Plough
Schering-Plough is a global science-based health care company with leading prescription, consumer and animal health products. Through internal research and collaborations with partners, Schering-Plough discovers, develops, manufactures and markets advanced drug therapies to meet important medical needs. Schering-Plough's vision is to earn the trust of the physicians, patients and customers served by its more than 32,000 people around the world. The company is based in Kenilworth, N.J., and its Web site is http://www.schering-plough.com.
-www.LupusMCTD.com-
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #22 on: May 07, 2007, 11:37:20 am » |
|
Overseas Co-Promotion of Actemra, a Treatment for Rheumatoid Arthritis
TOKYO, May 7, 2007 - Chugai Pharmaceutical Co., Ltd. [Head Office: Chuo-ku, Tokyo; President: Osamu Nagayama (hereinafter, Chugai)] announced today that under the terms of the license agreement signed with F. Hoffmann-La Roche [Head Office: Basel. Switzerland. Chairman and CEO: Franz B. Humer (hereinafter, Roche)] on the humanized anti-human IL-6 receptor monoclonal antibody Actemra®, it has decided not to exercise the opt-in right for co-promotion in the United States, Italy and Spain, and will co-promote the product with Roche in France, Germany and the United Kingdom.
In July 2003, Chugai and Roche signed a co-development and co-promotion license agreement granting Roche exclusive rights for Actemra®-related patents and trademark usage for the global market excluding Japan, South Korea and Taiwan. Under the agreement, Chugai holds the right for co-promotion in France, Germany and the United Kingdom, and the opt-in right for co-promotion in the United States, Italy and Spain
In France, Germany and the United Kingdom, where Chugai has its own marketing base, the two companies have started joint efforts to build the necessary organization and to plan marketing and promotion strategies. In the United States, Italy and Spain, however, Chugai decided not to exercise the opt-in right in those territories, in pursuit of maximizing the business value of Actemra® as early as possible, and in consideration of Chugai's mid-term strategy on overseas activities. Profits will be shared in France, Germany and the United Kingdom in proportion to each company's co-promotion effort.
Chugai and Roche have been advancing the co-development of Actemra® globally, and currently phase III clinical trial programs in rheumatoid arthritis are going on in 41 countries worldwide. Four out of five phase III clinical trials are scheduled to be reported by the end of the year, and Roche is planning to file for approval in Europe and in the United States in the latter part of 2007.
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #23 on: May 07, 2007, 11:52:42 am » |
|
Abbott Seeks U.S. and E.U. Regulatory Approvals for HUMIRA(R) (Adalimumab) as a Treatment for Juvenile Rheumatoid Arthritis
ABBOTT PARK, Ill., May 7,2007 -Abbott announced it has simultaneously submitted a supplemental Biologics License Application (sBLA) with the U.S. Food and Drug Administration (FDA) and a Type II Variation to the European Medicines Agency (EMEA) seeking approval to market HUMIRA(R) (adalimumab) as a treatment for juvenile rheumatoid arthritis (JRA) in the U.S. and juvenile idiopathic arthritis (JIA) in the European Union (EU). This filing marks the first pediatric indication sought for HUMIRA.
JRA, commonly referred to as JIA in the EU, is the most common form of arthritis in children and normally begins before the age of 16. Typical symptoms include persistent joint pain and stiffness that are usually worse in the morning or after a nap. The pain may limit movement of the affected joint, although many children will not complain of the pain. Walking with a limp is an early sign of JRA due to an affected knee. Depending on the severity of disease, JRA may affect bone development or cause growth abnormalities, such as one leg or arm growing longer than the other. The goal of treatment for JRA is to control inflammation, relieve pain, and preserve mobility and joint function, and ultimately prevent disease progression.
"If left untreated, JRA may slow a child's growth and cause disability into adulthood," said Daniel J. Lovell, MD, MPH, associate director, Special Treatment Center for Juvenile Arthritis, Cincinnati Children's Hospital Medical Center, Cincinnati. "HUMIRA may offer hope to children suffering with this unpredictable disease."
About HUMIRA JRA Clinical Study
The global filing is based on the results of a Phase III, 48-week study that included 171 children (4 to 17 years old) with polyarticular JRA, a form of arthritis affecting five or more joints, usually the same joints on both sides of the body. Additional data will be submitted from an ongoing open label extension study evaluating the long-term efficacy and safety of HUMIRA.
In the first part of the study, two groups of patients -- those taking methotrexate (MTX) and not taking MTX -- received HUMIRA subcutaneously every other week (EOW) for 16 weeks. Patient responses were measured using the American College of Rheumatology (ACR) Pediatric 30 score, which represents a 30 percent improvement in JRA signs and symptoms, such as the number of swollen joints with loss of motion, assessment of pain and level of disability. Children who showed a positive clinical response (n=133) entered the second part of the study and were randomized to receive HUMIRA or placebo for an additional 32 weeks or until disease flare. A flare was defined as a worsening of 30 percent or more in three of the six ACR Ped response variables, a minimum of two active joints, and no more than one indicator improving by 30 percent.
Children receiving HUMIRA, in the second part of the study, had significantly fewer disease flares than children on placebo, both without MTX (43 percent vs. 71 percent) and with MTX (37 percent vs. 65 percent). Additionally, twice as many children on HUMIRA achieved ACR Ped 70 compared to those on placebo (56 percent vs. 28 percent, respectively) at Week 48. The most common adverse events were infections (mostly mild upper respiratory) and injection site reactions. No tuberculosis or opportunistic infections were reported during this study. The adverse events observed in children were similar to those observed in adults in previous rheumatoid arthritis (RA) studies with HUMIRA.
HUMIRA is approved to treat adult patients with moderately to severely active rheumatoid arthritis. More than 180,000 patients worldwide are currently being treated with HUMIRA. HUMIRA is currently being studied in pediatric Crohn's disease, and Abbott plans to initiate trials for pediatric and adolescent psoriasis later this year.
"We are pleased by the submission of our first pediatric indication for HUMIRA," said Eugene Sun, M.D., vice president, Global Pharmaceutical Clinical Development at Abbott. "HUMIRA has already benefited thousands of adults suffering with RA, and this trial shows promise for children and families who are impacted by JRA."
Important Safety Information
Globally, prescribing information varies; refer to the individual country product label for complete information.
Serious infections, sepsis, tuberculosis (TB) and opportunistic infections, including fatalities, have been reported with the use of TNF- blocking agents, including HUMIRA. Many of these serious infections have occurred in patients also taking other immunosuppressive agents that in addition to their underlying disease could predispose them to infections. Infections have also been reported in patients receiving HUMIRA alone. Treatment with HUMIRA should not be initiated in patients with active infections. TNF-blocking agents, including HUMIRA, have been associated with reactivation of hepatitis B (HBV) in patients who are chronic carriers of this virus. Some cases have been fatal. Patients at risk for HBV infections should be evaluated for prior evidence of HBV infections before initiating HUMIRA. The combination of HUMIRA and anakinra is not recommended and patients using HUMIRA should not receive live vaccines.
More cases of malignancies have been observed among patients receiving TNF blockers, including HUMIRA, compared to control patients in clinical trials. These malignancies, other than lymphoma and non-melanoma skin cancer, were similar in type and number to what would be expected in the general population. There was an approximately 3.5 fold higher rate of lymphoma in combined controlled and uncontrolled open-label portions of HUMIRA clinical trials. The potential role of TNF-blocking therapy in the development of malignancies is not known. TNF-blocking agents, including HUMIRA, have been associated in rare cases with demyelinating disease and severe allergic reactions. Infrequent reports of serious blood disorders have been reported with TNF-blocking agents.
Worsening congestive heart failure (CHF) has been observed with TNF- blocking agents, including HUMIRA, and new onset CHF has been reported with TNF-blocking agents. Treatment with HUMIRA may result in the formation of autoantibodies and rarely, in development of a lupus-like syndrome.
The most frequent adverse events seen in the placebo-controlled clinical trials in adults with rheumatoid arthritis (HUMIRA vs. placebo) were injection site reactions (20 percent vs. 14 percent), upper respiratory infection (17 percent vs. 13 percent), injection site pain (12 percent vs. 12 percent), headache (12 percent vs. 8 percent), rash (12 percent vs. 6 percent) and sinusitis (11 percent vs. 9 percent). Discontinuations due to adverse events were 7 percent for HUMIRA and 4 percent for placebo. As with any treatment program, the benefits and risks of HUMIRA should be carefully considered before initiating therapy.
In HUMIRA clinical trials for ankylosing spondylitis, psoriatic arthritis and Crohn's disease, the safety profile for adult patients treated with HUMIRA was similar to the safety profile seen in adult patients with rheumatoid arthritis.
About HUMIRA
HUMIRA is the only fully human monoclonal antibody approved for the treatment of rheumatoid arthritis (RA), psoriatic arthritis (PsA), and ankylosing spondylitis (AS) in the U.S. and Europe and Crohn's disease in the U.S. HUMIRA resembles antibodies normally found in the body. It works by blocking tumor necrosis factor alpha (TNF-alpha), a protein that when produced in excess, plays a central role in the inflammatory responses of many immune- mediated diseases. Clinical trials are currently under way evaluating the potential of HUMIRA in other autoimmune diseases.
In the U.S., HUMIRA is approved by the FDA for reducing signs and symptoms, inducing major clinical response, inhibiting the progression of joint structural damage, and improving physical function in adult patients with moderately to severely active RA. HUMIRA is indicated for reducing the signs and symptoms of active arthritis, inhibiting the progression of structural damage and improving physical function in patients with psoriatic arthritis. HUMIRA can be used alone or in combination with methotrexate or other disease-modifying anti-rheumatic drugs (DMARDs). HUMIRA is also approved for reducing signs and symptoms in patients with active AS. Earlier this year, HUMIRA was approved for reducing the signs and symptoms and inducing and maintaining clinical remission in adults with moderately to severely active Crohn's disease who have had an inadequate response to conventional therapy, and reducing the signs and symptoms and inducing clinical remission in these patients if they have also lost response to or are intolerant to infliximab.
In Europe, HUMIRA, in combination with methotrexate (MTX), is indicated for the treatment of moderate to severe, active RA in adult patients when the response to disease-modifying anti-rheumatic drugs (DMARDs) including MTX has been inadequate, and for the treatment of severe, active and progressive RA in adults not previously treated with MTX. HUMIRA can be given as monotherapy in case of intolerance to MTX or when continued treatment with MTX is inappropriate. HUMIRA has been shown to reduce the rate of progression of joint damage as measured by x-ray and to improve physical function, when given in combination with MTX.
Additionally, HUMIRA is indicated for the treatment of active and progressive PsA in adults when the response to previous DMARD-therapy has been inadequate and for the treatment of severe, active AS in adults who have had an inadequate response to conventional therapy.
Abbott's Commitment to Immunology
Abbott is focused on the discovery and development of innovative treatments for immunologic diseases. The Abbott Bioresearch Center, founded in 1989 in Worcester, Mass., United States, is a world-class discovery and basic research facility committed to finding new treatments for immune- mediated diseases.
In April 2007, Abbott announced the opening of Abbott Biotechnology Limited (ABL), its new state-of-the-art biologics manufacturing facility in Puerto Rico to support the long-term supply of HUMIRA. The new facility is the main manufacturing site for supplying HUMIRA to patients in the U.S.
More information about HUMIRA, including full prescribing information, is available on the Web site http://www.humira.com/ or in the United States by calling Abbott Medical Information at 1-800-633-9110.
About Abbott
Abbott is a global, broad-based health care company devoted to the discovery, development, manufacture and marketing of pharmaceuticals and medical products, including nutritionals, devices and diagnostics. The company employs 65,000 people and markets its products in more than 130 countries.
www.LupusMCTD.com
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #24 on: June 29, 2007, 07:45:38 pm » |
|
Doctors overestimate RA patient disability
Rheumatologists substantially overestimate the physical disability of patients with rheumatoid arthritis, according to a U.S. study.
Researchers at the University of South Florida College of Medicine and James A. Haley Veterans' Hospital, both in Tampa, Fla., found a clear physician-patient difference in assessment of the patients' functional disability.
The rheumatologists consistently rated their rheumatoid arthritis patients' degree of difficulty in performing activities of daily living, such as walking, dressing and eating, higher than the patients themselves, according to the study published in the Journal of Rheumatology.
"We flunked," co-first author Dr. John D. Carter said in a statement. "The very physicians deemed to be experts in rheumatoid arthritis failed to make the grade when it came to determining their patients' functional status."
The discrepancy is important to correct because patients can rely on these assessments for their livelihood or other necessities to perform activities of daily living, according to Carter.
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #25 on: September 23, 2007, 10:50:45 am » |
|
Death in Gene Therapy Treatment Is Still Unexplained
A federal committee concluded yesterday that it was too early to tell whether an experimental gene therapy treatment for rheumatoid arthritis contributed to the death of a 36-year-old woman in July.
But the committee, set up by the National Institutes of Health to help oversee gene therapy clinical trials, raised questions about the process used to enroll the woman in the study. And the womans husband said he thought his wife should not have been recruited.
The biggest question I have is would my wife still be alive today if she hadnt participated in this study? Robb Mohr of Taylorville, Ill., said in brief, tearful remarks about his wife, Jolee. I have it in my heart that shed still be here.
If Ms. Mohrs death is eventually tied to the gene therapy, it could set back a field that has already had its share of failures and black eyes, including the death in 1999 of a teenager, Jesse Gelsinger, in a gene therapy test at the University of Pennsylvania.
Jolee Mohr, who had a 5-year-old daughter, died on July 24 at the University of Chicago Medical Center, three weeks after trillions of genetically engineered viruses were injected into her right knee as a test of an experimental treatment for rheumatoid arthritis. The type of virus used as a gene carrier has widely been considered safe and is being used in 35 other trials.
Autopsy data presented at the committee meeting yesterday in Bethesda, Md., suggested that the main cause of death was a fungal infection, histoplasmosis, that had gone out of control, destroying her organs. Ms. Mohr also suffered from internal bleeding, with a pool of blood in her abdomen that was so large that it displaced her kidneys and other organs.
The results indicated that the virus did not directly kill her. But a major question for the committee, known as the Recombinant DNA Advisory Committee, was whether the gene therapy suppressed her immune system, allowing the fungus to run wild. The gene therapy was meant to cause cells in her knee joint to produce an anti-inflammatory protein identical to the one in Enbrel, a widely used arthritis drug. Enbrel can leave patients more susceptible to infections.
But Ms. Mohr was also taking regular injections of Humira, a drug similar to Enbrel that has also been linked to infections, including histoplasmosis. She was also on two other immune-suppressing drugs.
Studies found that the genetically engineered virus had spread to Ms. Mohrs liver and spleen. That raised the possibility that the immune-suppressing protein was produced outside the joint.
H. Stewart Parker, the president of Targeted Genetics, said after the meeting that the levels of virus in the liver and spleen had been tiny, strengthening the companys view that its therapy was not at fault.
Referring to adeno-associated virus, the type used in the gene therapy, Ms. Parker said, Anybody who knows anything about A.A.V. would be shocked if it had anything to do with anything.
The company has always said that the injection into the joint produces minuscule amounts of immune-suppressing protein compared with taking a drug like Humira through injection into the bloodstream.
Some committee members seemed to agree. It certainly would not have killed the patient, Dr. Hildegund C. J. Ertl, a vaccine researcher at the Wistar Institute in Philadelphia, said of the virus leak to the liver and spleen.
But Alan C. Milstein, a lawyer for Mr. Mohr, said after the meeting that it was suspicious that Ms. Mohr, who had been taking Humira for a long time, had a problem only after receiving the gene therapy injection.
Testing continues on Ms. Mohrs blood and other tissues. But some panel members said the role of the gene therapy in Ms. Mohrs death might never be definitively determined.
Some members said Ms. Mohr might not have been given enough time to consider whether to enroll in the trial. And they said the fact that she was recruited by her rheumatologist might have led her to believe she would benefit from the trial, even though its main purpose was to gather information.
Mr. Mohr said it was still beyond my belief that his wife had been recruited, since, he said, she had never missed work because of her arthritis. If she were still alive and walked into the room, he told the panel, besides gawking at her beauty you would never know anything was wrong with her.
Moreover, the autopsy showed no active disease in the right knee joint, though some arthritis specialists said that such active disease could be hard to detect when a patient was taking drugs. Ms. Mohr had received 10 injections of steroids into that knee in the last few years, a sign that her other drugs had not provided full relief. She also had surgery late last year for problems in her toes caused by the arthritis.
Dr. Arthur W. Nienhuis, president of the American Society of Gene Therapy, told the committee that researchers in the field should pay more attention to informed consent.
No regulations were violated in this case, Dr. Nienhuis said. But perhaps we should hold ourselves to a higher standard. |
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #26 on: September 23, 2007, 12:05:53 pm » |
|
A Breakthrough in Joint Pain
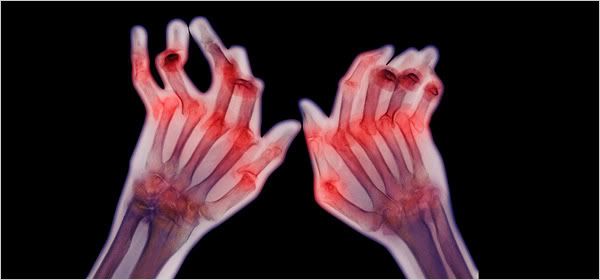
Revolutions are rare in the management of chronic disease, which tends to be a matter of incremental progress. But over the past decade, patients with rheumatoid arthritis have seen advances in treatment that most could barely have imagined. A new class of drugs called biologic response modifiers has transformed the lives of countless R.A. sufferers, so much so that many have been able to return to active, rich lives.
But the biologics, as they are often called, do not work for all patients, and rheumatologists still are struggling to figure out who is most likely to benefit. The drugs must be taken by injection, and the side effects some discovered only recently can be significant, even dangerous. Whether to take biologic response modifiers is perhaps the most important question facing rheumatoid arthritis patients today, and it is making for Hobbesian choices.
Biologic response modifiers slow or halt the progression of the disease by blocking the action of cytokines, substances that promote inflammation in joints and activate the process of cartilage destruction. The first cytokine successfully targeted by medication is tumor necrosis factor, or TNF-alpha; approved medications include adalimumab (Humira), infliximab (Remicade) and etanercept (Enbrel).
Biologic response modifiers, often given in combination with methotrexate or another so-called disease-modifying anti-rheumatic drug, are now the gold standard in rheumatoid arthritis treatment. Yet biologics do not work for everyone not by a wide margin. Roughly one-third of R.A. patients experience significant improvement on anti-TNF-alpha drugs, and a third show some improvement. But the remainder are unaffected; many patients do not respond even to the most aggressive treatments available.
Even those who do respond must first muddle through a period of trial and error before finding the right medication. Some people will respond to one and not another, or fail two and still respond to a third, said Dr. Vibeke Strand, a rheumatologist at Stanford University. Its very hard to say.
For all the uncertainty, biologics are enormously expensive: these treatments can cost $15,000 to $30,000 a year. And because they suppress the immune system, the drugs carry significant risks. Recent studies have shown that TNF inhibitors can greatly increase the chances of developing serious infections and some cancers. According to a 2006 survey by rheumatology researchers at the Mayo Clinic, rheumatoid arthritis patients taking TNF inhibitors were 2.2 times more likely than a placebo group to develop such infections as pneumonia and tuberculosis, and 3.3 times more likely to develop certain types of cancer.
Far more rarely, scientists have documented increased rates of multiple sclerosis, lupus and liver damage among patients taking biologics. Yet it is difficult to know to what extent the drugs are to blame. Whether using biologics or not, R.A. patients tend to suffer more infections and other conditions than people without the disease. The side effects may result from an unfortunate synergy between the first-line therapeutics, like methotrexate and leflunomide, and the newer drugs, rather than the biologics themselves. Or it may be simply that the sickest patients also are the ones most likely to receive TNF inhibitors.
Amid the questions of risk, a positive but little-noted effect of biologics has also emerged. While people with rheumatoid arthritis are more likely to get cardiovascular disease (including congestive heart failure) and to die of it than the general population, preliminary research shows that TNF inhibitors may actually provide some cardiovascular protection.
At the moment, most researchers agree that the benefits of biologics far outweigh the risks.
What they have been able to do, both to prevent disability and to improve physical function, is amazing, just amazing, said Dr. Strand. For many patients, the drugs have accomplished something rare in medicine: they have moved patients from suffering to something resembling normalcy. A Breakthrough in Joint Pain
By ALIYAH BARUCHIN
Revolutions are rare in the management of chronic disease, which tends to be a matter of incremental progress. But over the past decade, patients with rheumatoid arthritis have seen advances in treatment that most could barely have imagined. A new class of drugs called biologic response modifiers has transformed the lives of countless R.A. sufferers, so much so that many have been able to return to active, rich lives.
But the biologics, as they are often called, do not work for all patients, and rheumatologists still are struggling to figure out who is most likely to benefit. The drugs must be taken by injection, and the side effects some discovered only recently can be significant, even dangerous. Whether to take biologic response modifiers is perhaps the most important question facing rheumatoid arthritis patients today, and it is making for Hobbesian choices.
Biologic response modifiers slow or halt the progression of the disease by blocking the action of cytokines, substances that promote inflammation in joints and activate the process of cartilage destruction. The first cytokine successfully targeted by medication is tumor necrosis factor, or TNF-alpha; approved medications include adalimumab (Humira), infliximab (Remicade) and etanercept (Enbrel).
Biologic response modifiers, often given in combination with methotrexate or another so-called disease-modifying anti-rheumatic drug, are now the gold standard in rheumatoid arthritis treatment. Yet biologics do not work for everyone not by a wide margin. Roughly one-third of R.A. patients experience significant improvement on anti-TNF-alpha drugs, and a third show some improvement. But the remainder are unaffected; many patients do not respond even to the most aggressive treatments available.
Even those who do respond must first muddle through a period of trial and error before finding the right medication. Some people will respond to one and not another, or fail two and still respond to a third, said Dr. Vibeke Strand, a rheumatologist at Stanford University. Its very hard to say.
For all the uncertainty, biologics are enormously expensive: these treatments can cost $15,000 to $30,000 a year. And because they suppress the immune system, the drugs carry significant risks. Recent studies have shown that TNF inhibitors can greatly increase the chances of developing serious infections and some cancers. According to a 2006 survey by rheumatology researchers at the Mayo Clinic, rheumatoid arthritis patients taking TNF inhibitors were 2.2 times more likely than a placebo group to develop such infections as pneumonia and tuberculosis, and 3.3 times more likely to develop certain types of cancer.
Far more rarely, scientists have documented increased rates of multiple sclerosis, lupus and liver damage among patients taking biologics. Yet it is difficult to know to what extent the drugs are to blame. Whether using biologics or not, R.A. patients tend to suffer more infections and other conditions than people without the disease. The side effects may result from an unfortunate synergy between the first-line therapeutics, like methotrexate and leflunomide, and the newer drugs, rather than the biologics themselves. Or it may be simply that the sickest patients also are the ones most likely to receive TNF inhibitors.
Amid the questions of risk, a positive but little-noted effect of biologics has also emerged. While people with rheumatoid arthritis are more likely to get cardiovascular disease (including congestive heart failure) and to die of it than the general population, preliminary research shows that TNF inhibitors may actually provide some cardiovascular protection.
At the moment, most researchers agree that the benefits of biologics far outweigh the risks.
What they have been able to do, both to prevent disability and to improve physical function, is amazing, just amazing, said Dr. Strand. For many patients, the drugs have accomplished something rare in medicine: they have moved patients from suffering to something resembling normalcy. |
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #27 on: October 18, 2007, 12:42:41 pm » |
|
Fatigue in rheumatoid arthritis: from apathy to action Professor of Rheumatology and Nursing University of the West of England, Rheumatology Unit, Bristol Royal Infirmary, Bristol BS2 8HW, UK.
Fatigue is a common problem in rheumatoid arthritis (RA), experienced by the majority of patients, with fatigue scores that are often higher than pain scores [1,2]. Despite this, patients feel fatigue has been largely ignored by clinicians. This article provides a personal overview of the journey of RA fatigue from nonexistence to hot topic and looks toward a time when fatigue might return to nonexistence because it is routinely and effectively managed.
Importance of fatigue ChooseTop of pageImportance of fatigue <<Meaning of fatigueMechanisms of fatigueMeasurement of fatigueMultiple end points for f...Management of fatigueIn the clinic situationConclusionFuture perspectiveBibliography
The journey for fatigue from nonexistence to hot topic was largely prompted by patients. In 2002, patients attended a meeting of the international group Outcome Measurement in Rheumatology Clinical Trials (OMERACT) and were invited to discuss the ACR Core set for RA clinical trials [3].
They said it was unimpressive as it omitted symptoms important to them. This led to qualitative research in the UK and Sweden, exploring what were the important outcomes for patients [4,5]. Fatigue was spontaneously generated and subsequent research revealed that patients rate it as more important than joint swelling or pain [6,7]. Patients said fatigue was important because of its impact on their lives and research confirms that fatigue distinguishes between quality-of-life profiles [8]. A greater understanding of the way in which fatigue affects quality of life was therefore needed.
Meaning of fatigue ChooseTop of pageImportance of fatigueMeaning of fatigue <<Mechanisms of fatigueMeasurement of fatigueMultiple end points for f...Management of fatigueIn the clinic situationConclusionFuture perspectiveBibliography
Qualitative research exploring RA fatigue revealed three major themes [9]. First, fatigue in RA is overwhelming and different from normal tiredness, being experienced as extreme weariness, weight or heaviness, and complete wipe-out (when the patient has to stop altogether). Patients describe cognitive and emotional components, such as an inability to think straight and tearfulness, and say fatigue is unearned, unpredictable and unresolving.
Second, the consequences of fatigue permeate every sphere of life, with far-reaching effects on physical activities, emotions, relationships and roles.
Third, patients report that their ability to manage fatigue is limited but that they rarely receive professional support. Most patients were not asked by their rheumatologist about fatigue, and when they raised the issue, patients felt it was dismissed. Anecdotally, rheumatologists tell patients fatigue is just part of their disease perhaps assuming the mechanism to be inflammation.
Mechanisms of fatigue ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigue <<Measurement of fatigueMultiple end points for f...Management of fatigueIn the clinic situationConclusionFuture perspectiveBibliography
Mechanisms driving fatigue in RA may be biochemical (inflammation and anemia), physiological (muscle deconditioning, excess effort expended due to disability and poor sleep) or psychosocial (stress, anxiety, depression and low social support). However, evidence for associations between these single variables and RA fatigue yields contradictory results, apart from some consistency in the lack of association with C-reactive protein, anemia and age. It is probable that a combination of variables provides the driving mechanism for RA fatigue, and here there is more consistency, with various explanatory models usually including pain, function and psychosocial variables [1,10,11].
There are several problems with establishing a clear explanatory model for RA fatigue. First, there are many candidate variables to be explored and it appears that no study has measured all of these in a prospective study. Second, the explanatory model is likely to be a complex, multicausal pathway that is cyclical, with events fuelling each other (e.g., pain causing stress, leading to fatigue, which increases sensitivity to pain and stress). It is likely that this pathway will comprise different components for different patients at different points in their disease trajectory (with implications for interventions). Finally, we must be able to measure RA fatigue accurately.
Measurement of fatigue ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigueMeasurement of fatigue <<Multiple end points for f...Management of fatigueIn the clinic situationConclusionFuture perspectiveBibliography
A systematic search of the literature revealed 23 different fatigue scales used to measure RA fatigue between 1980 and 2004 [12]. However, a review of the published evidence for their validity, reliability and sensitivity suggested only six scales had reasonable evidence of validation in an RA population. Only one was designed for RA patients, and even the frequently used fatigue visual analogue scale (VAS) was neither standardized nor validated for use in RA (only three of the 26 VAS used were identical). Researchers in the UK and The Netherlands are currently developing and validating VAS and multidimensional fatigue scales specific to RA, and will hopefully include validation in the USA and Europe [13]. The development of multi-dimensional scales will allow the identification of different end points following fatigue interventions.
Multiple end points for fatigue interventions ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigueMeasurement of fatigueMultiple end points for f... <<Management of fatigueIn the clinic situationConclusionFuture perspectiveBibliography
As fatigue has multidimensional effects on people with RA [9], there is the potential to alter these differentially with different interventions. For example, many patients have low self-efficacy for managing fatigue [11], and enhancing self-efficacy might therefore form the focus of an intervention. Other patients may report a lessening of the effects of fatigue in their lives, even if their global fatigue score remains unchanged. For example, they might be more physically active despite the same level of fatigue, or they may be able to stay awake in company rather than fall asleep. Although medication to reduce RA fatigue would be helpful, it may not be desired or appropriate for all patients, therefore multiple approaches to managing fatigue should be developed.
Management of fatigue ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigueMeasurement of fatigueMultiple end points for f...Management of fatigue <<In the clinic situationConclusionFuture perspectiveBibliography
There is increasing evidence that the use of biologic agents and DMARDs can give significant improvements in RA fatigue [14,15] and it is suggested this is through an association with changes in pain and mood, rather than inflammatory activity [2]. These medications have potentially serious side effects, are expensive and patients may have limited access; therefore, if fatigue is present in a patient whose RA is otherwise well controlled, medication changes might not be the appropriate intervention.
In a systematic review of nonpharmacological interventions for fatigue, only two randomized controlled trials were identified in RA [16]. A randomized, controlled trial of home aerobic training demonstrated a trend toward fatigue improvement. However, a randomized, controlled trial of cognitivebehavioral therapy (CBT) in early RA patients at risk of psychological distress demonstrated significant improvement in fatigue [17]. CBT addresses the thoughts (or beliefs) and feelings that influence behaviors and uses individualized problem-solving, goal-setting and cognitive restructuring to help patients change behavior. Such an approach is currently being tested in the UK in patients with high fatigue levels but who are otherwise unselected.
Clearly there are other interventions that still need testing. For example, what are the effects of single components of self-management such as pacing and planning, or joint protection? Can self-management interventions using CBT approaches be delivered by members of the rheumatology team (with suitable training) rather than by specialized clinical psychologists? High-quality studies on reversing deconditioning or to enhance exercise should be carried out, as well as studies that address depression, social support or nonrestorative sleep.
Since patients raised the issue at OMERACT in 2002, RA fatigue has received a great deal of interest and has become something of a hot topic, which demonstrates the power of the patient voice. Research grants have been awarded and studies are under way internationally in a range of areas. After reviewing the available evidence at OMERACT 2006, an international consensus was reached that fatigue should now be measured in all RA clinical trials whenever possible [18]. This will help to further drive the efforts to develop and test useful interventions.
In the clinic situation ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigueMeasurement of fatigueMultiple end points for f...Management of fatigueIn the clinic situation <<ConclusionFuture perspectiveBibliography
Meanwhile, what should the busy clinician do, when a patient with RA reports fatigue? Simply acknowledging and discussing the problems that fatigue causes may validate fatigue as a genuine symptom for patients. Exploring biochemical, physiological and psychosocial causes might help guide thoughts on potential interventions. For example, one patient complained of fatigue affecting her ability to work in the office, but eventually it was revealed that she did not eat until the evening persuading her to eat some breakfast and lunch had a dramatic effect on her fatigue. Referral to members of the multidisciplinary team to assist in managing this distressing symptom is almost certain to be welcomed by the patient.
Conclusion ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigueMeasurement of fatigueMultiple end points for f...Management of fatigueIn the clinic situationConclusion <<Future perspectiveBibliography
Fatigue is a common problem that distresses patients with RA and impacts on their quality of life. Many research avenues are being explored, including issues around mechanisms, measurement and management. Although the search for effective pharmacological and nonpharmacological interventions is under way, there is currently only evidence for DMARDs, biologic agents and CBT. These may not be appropriate or available to all patients; therefore until more evidence on effective interventions appears, busy clinicians should consider referring patients to any member of their multidisciplinary team who has, or would be willing to develop, a special interest in the self-management of fatigue.
Future perspective ChooseTop of pageImportance of fatigueMeaning of fatigueMechanisms of fatigueMeasurement of fatigueMultiple end points for f...Management of fatigueIn the clinic situationConclusionFuture perspective <<Bibliography
Over the next 510 years, given the current level of patient, clinician and researcher interest in RA fatigue, evidence on measurement, mechanisms and management should steadily accumulate, facilitating the development of an evidence-based treatment algorithm. Within the next decade, fatigue will be routinely discussed and assessed during clinic consultations, the driving mechanism for the individual patient identified, and the patient offered an appropriate intervention using the treatment algorithm. The intervention might be pharmacological or nonpharmacological but will automatically include referral to a member of the multidisciplinary team with a special interest in enhancing fatigue self-management. Then, once again, fatigue will become nonexistent as it becomes routinely managed, in the same way that pain is routinely addressed.
Executive summary Importance of rheumatoid arthritis fatigue Fatigue is common and may be more severe than pain. Meaning of rheumatoid arthritis fatigue Fatigue is overwhelming, uncontrolled and ignored by clinicians. Mechanisms of fatigue Biochemical, physiological and psychosocial elements may contribute different amounts at different times for individual patients. Measurement of fatigue Scales should be selected carefully few are validated for rheumatoid arthritis, new scales are being developed. Multiple end points for fatigue interventions If severity cannot be changed, other outcomes might include improved quality of life, more physical activity but no increase in fatigue, or greater self-efficacy for managing fatigue. Management of fatigue There is evidence for biologic agents, DMARDs and cognitivebehavioral therapy at present. In the clinic situation Acknowledge, discuss, assess, investigate, treat and arrange support with self-management. [/size] |
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #28 on: February 28, 2008, 03:40:47 pm » |
|
Video link~
Kathleen sat down with Access Hollywoods Billy Bush and opened up about her disease rheumatoid arthritis and her incredibly honest book of memoirs, a New York Times best seller, "Send Yourself Roses".http://www.accesshollywood.com/article/8563/?__dst=rss%7Cah_Latest
|
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
Adminஐﻬ
|
 |
« Reply #29 on: May 24, 2008, 07:53:54 pm » |
|
Arthritis drug trail
Sufferers of arthritis are being asked to take part in a drugs trial.
Fifty people from St Albans are being invited to take part in the clinical study which is aiming to reduce death rates from heart attacks and strokes for people suffering from rheumatoid arthritis (RA).
The five year trail is to see 3,800 people nation-wide take part by testing a new cholesterol-busting drug called statins.
The local research team is led by consultant rheumatologist Dr Adam Young at St Albans City Hospital.
"It has been known for some time that there is a link between rheumatoid arthritis and cardio-vascular mortality," said Dr Young.
"Statins lead to a reduction of cardiovascular death rates by reducing cholesterol and possibly inflammation.
"If this trial works as expected, we could be looking at a reduction of the absolute risk of cardiovascular death rate in RA patients by ten to 15 per cent, or the relative risk by 35 to 40 per cent, which is significant."
The trail is currently recruiting RA patients over the age of 50 and or if they have suffered for more than ten years.
More information can be found at the RA trial website: http://www.dgoh.nhs.uk/tracera or by contacting 01612 755639. |
|
|
|
|
 Logged
Logged
|
 I look normal, as I have an "Invisible Illness". You can not catch it, you can not see it. It's called Lupus.My body is attacking itself on the inside.  www.LupusMCTD.com www.LupusMCTD.com Represents: 1) We are patients helping researchers build a future for the lives of others... 2) Where HOPE is a WORK In Progress 3) Pay It Forward~Giving Back To The Future Lupus/MCTD Patients |
|
|
|
|
|



